Real-Time Monitoring: Impact on Patient Pre-Visit Workflows
Clinic Operations & Workflow Automation
Clinic Operations & Workflow Automation
Real-time monitoring cuts pre-visit wait times, reduces data errors, automates intake tasks, and boosts staff productivity and ROI.
Real-time monitoring cuts pre-visit wait times, reduces data errors, automates intake tasks, and boosts staff productivity and ROI.

Real-time monitoring is transforming how clinics handle pre-visit workflows, cutting down inefficiencies and improving patient care. It reduces wait times, minimizes errors, and saves staff hours by automating tasks like data entry and insurance verification. For example, clinics using AI-powered systems have seen patient wait times drop by 82% and data entry errors reduced to 0.3%. These tools also streamline processes, allowing clinics to handle more patients without overburdening staff.
Key benefits include:
Time savings: Clinics save hours daily by automating manual tasks.
Improved accuracy: Data entry error rates drop significantly.
Shorter wait times: Patients experience faster service, enhancing satisfaction.
Higher ROI: Some clinics report over 1,300% return on investment.
Research Findings: Real-Time Monitoring Benefits for Pre-Visit Workflows
Time Savings and Efficiency Improvements
Real-time monitoring systems have made a noticeable impact on clinic operations, especially in terms of time management and efficiency. For example, the University of Michigan Kellogg Eye Center implemented a passive RFID real-time locating system in their glaucoma clinic between January and July 2018. Across 1,972 patient visits, the system shaved 2.9 minutes off technician process times per patient, saving around 156 minutes daily. This efficiency boost allowed the clinic to increase its daily patient load from 51.9 to 58.4, all without extending overall wait times.
Similarly, MD Anderson Cancer Center's Department of Gastrointestinal Radiation Oncology adopted real-time EMR tracking for 556 consultation visits between May 2019 and September 2020. This initiative reduced the median cycle time by 21%, cutting it from 91 minutes to 72 minutes. Cumulative waiting times dropped by 64%, going from 45 minutes to just 16 minutes. Additionally, the proportion of visits exceeding two hours fell from 22% to 0%.
These improvements highlight how real-time monitoring not only saves time but also enhances the overall efficiency of pre-visit workflows.
Better Data Accuracy and Workflow Reliability
Accurate data is crucial in creating reliable workflows, and real-time systems have delivered impressive results. A dermatology practice operating across three offices introduced a HIPAA-compliant AI intake system to process over 300 forms weekly. Within just 30 days, this system reduced data entry error rates from 3.8% to 0.3%, improved pre-visit insurance verification rates from 0% to 94%, and cut manual data entry time from 2–3 hours per day to just 15 minutes. The system utilized OCR and a natural language processing engine tailored for medical terminology, ensuring any low-confidence data entries were flagged for staff review.
In another example, Amplify Care in Ontario implemented a Business Automation Workflow platform to streamline e-Referrals and fax systems. By adding automated retry logic in March 2023, they reduced fax failure rates from 37.7% to 9.9%, achieving a 98.7% successful delivery rate across 4,504 e-Faxes for 4,132 patients.
These advancements in data accuracy not only minimize errors but also reduce delays, making pre-visit processes more dependable.
Fewer Pre-Visit Delays
Real-time monitoring has also proven effective in cutting down pre-visit delays. The dermatology practice mentioned earlier achieved an 82% reduction in patient wait times, bringing the average wait from 22 minutes to just 4 minutes. This was accomplished by completing data entry and insurance verification ahead of time using digital intake links sent to patients 48 hours before their appointments.
In radiation oncology, real-time EMR status boards improved communication among nursing staff, residents, and attending physicians. By clarifying roles and eliminating redundant tasks like repeated history-taking, these systems helped streamline the workflow from registration to consultation.
Technologies That Enable Real-Time Monitoring
AI-Powered Document Management
AI has transformed document management by automating processes like fax triage and referral tracking. Using OCR (Optical Character Recognition) and NLP (Natural Language Processing), these systems extract data from handwritten forms, insurance cards, and faxes with accuracy rates reaching up to 99.2%.
Take Penn Medicine, for example. In November 2025, they rolled out "coordn8", an AI-driven system designed for fax processing and digital consent. This tool processed 3,000 faxes daily, saving 8,500 staff hours over 18 months. It also slashed the time needed to obtain patient signatures by 85% through text-based eDisclosure. Jency Daniel highlighted the impact:
"Reducing processing time allows staff to focus on more patient-facing activities and results in higher job satisfaction. Vacations or sick days won't slow the process down anymore."
A similar success story unfolded in January 2026 when a major U.S. health insurer partnered with Alithya. By applying Small Language Models, they automated 97% of fax submissions, achieved 80% straight-through processing, and saved $2.2 million annually.
Platforms like Diagna's FAXFlo bring these capabilities to specialty clinics. FAXFlo automatically receives, reads, categorizes, and routes incoming faxes. It also extracts key patient details, links documents to the correct EMR record, and saves over four hours of staff time daily with over 98% accuracy.
These AI-powered tools lay the groundwork for further automation, including scheduling and seamless EMR integration.
Automated Scheduling and Reminders
While AI streamlines document handling, automated scheduling tools improve patient readiness and reduce no-shows. Digital intake engines send secure links to patients, allowing them to complete demographics, verify insurance, and answer condition-specific questions from the comfort of their homes. Responses sync directly with the EHR, and research shows that 77% of patients prefer this digital approach for completing pre-visit forms.
Real-time wait tracking systems take patient convenience a step further. By providing updates on queue positions and predicting wait times with over 94% accuracy via SMS, these platforms ease patient anxiety and reduce walk-outs. They can also send apology messages for delays and follow-up reminders based on diagnoses. With no app downloads required, SMS-based systems have adoption rates exceeding 60%.
Additionally, automated systems save staff time by handling routine tasks like notifying patients of lab results and managing callbacks, freeing up around 10 hours per week.
EMR Integration
Once data is captured and appointments are scheduled, EMR integration ensures everything flows smoothly into patient care. Modern systems use HL7 FHIR standards and APIs to securely synchronize data.
This two-way synchronization means information from digital forms, insurance verifications, and referrals automatically updates in the EMR. Staff no longer need to re-enter data, which ensures patient charts are complete and ready when the visit begins. As Solum Health explains:
"Clean data posts to the EHR and the scheduling and billing queues through API integration. On arrival, the chart is complete, the front desk sees what is pending, and the visit starts on time."
Between May 2022 and December 2023, Amplify Care tested a system in Ontario that integrated an eReferral platform with fax-reliant receivers using HL7 FHIR. The platform processed 4,504 eFaxes for 4,132 unique patients. By March 2023, new retry logic reduced fax failure rates from 37.7% to 9.9%, with 98.7% of eFaxes successfully delivered after retries.
Diagna offers EMR integration that works with any system, allowing clinics to maintain their current workflows. This flexibility ensures that automated document processing and referral tracking integrate seamlessly, delivering real-time updates and fully completed charts without disrupting existing processes.
Making Clinical AI Work: Workflow-Native Automation and the Future of Healthcare Efficiency
Clinical and Operational Results from Real-Time Monitoring
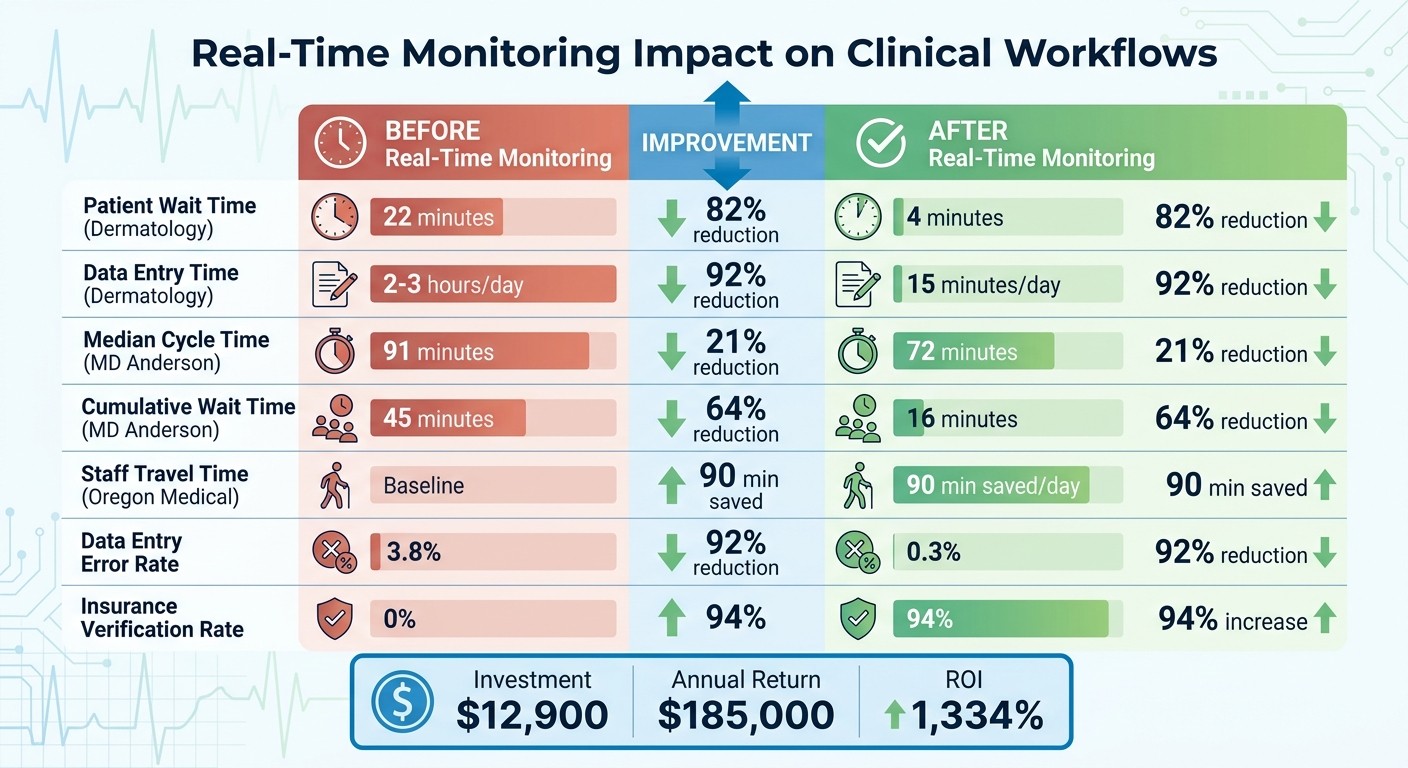
Real-Time Monitoring Impact on Clinical Workflows: Before vs After Results
The efficiency gains from real-time monitoring are making a noticeable difference in healthcare, improving both operations and clinical outcomes across various settings.
Staff Time Savings and Increased Productivity
Real-time monitoring is reshaping how clinics operate. For instance, Oregon Medical Group implemented a Real-Time Location System (RTLS) that allowed patients to self-room after registration. This eliminated the need for staff to shuttle patients between waiting areas and exam rooms. Steve Liu, their Director of IT, shared:
"The efficiencies we've gained from using CenTrak's RTLS system have been quite incredible. Patients are getting more time with their care team while also experiencing a decrease in appointment wait times."
Another example comes from a dermatology practice with eight providers across three locations. By automating data entry, they slashed the time spent on this task by 92%, going from 2–3 hours daily to just 15 minutes per location. The practice administrator highlighted the financial impact:
"Our front desk staff were spending half their day typing data from forms into Athenahealth. Now the AI handles it before the patient even walks in. The $7,500 investment paid for itself in the first month."
At MD Anderson Cancer Center, the Department of Gastrointestinal Radiation Oncology saw impressive results from using real-time tracking in their Epic EMR. This system eliminated duplicate tasks and clarified nursing roles for 556 consults between 2019 and 2020. As a result, visits lasting over two hours dropped from 22% to 0%, significantly cutting cycle times and patient waiting periods.
These changes free up staff to focus on what really matters - patient care - while making the overall experience more seamless.
Better Patient Satisfaction and Care Quality
Improved workflows and shorter wait times are directly enhancing patient satisfaction. The dermatology practice mentioned earlier saw its Google review rating rise from 4.1 to 4.6 stars, while negative comments about wait times dropped by 78%. This was largely due to the reduction in patient wait times to just four minutes.
Another success story comes from the pediatric therapy clinic Always Keep Progressing, which reduced its patient onboarding process by 99% - from two weeks to same-day completion. Gabriela Castro, the Clinic Manager, explained how this change has positively impacted their operations:
"Before Solum, it was almost a full day on the phone. Now we have more time to focus on other things. Definitely it's been so helpful."
Patients also appreciated the simpler process. Castro added:
"The feedback from the patients is like kind of easier for them. Just with that link, and then if they have any question they can just ask for an in-person representative."
Additionally, the clinic automated all insurance verifications, eliminating last-minute surprises and reducing the need to reschedule due to coverage issues.
These operational upgrades not only enhance care but also lead to financial rewards.
Financial Impact and ROI
The financial benefits of real-time monitoring are undeniable. For example, the dermatology practice invested $12,900 in the first year and generated a $185,000 annual impact, achieving an ROI of 1,334%. They also reduced data entry error rates from 3.8% to 0.3%.
On a larger scale, Atrium Health Wake Forest reported a $10 million total benefit from Enterprise Location Services, while Piedmont Healthcare saved $500,000 annually by standardizing asset management and cutting rental and maintenance costs. Meanwhile, an outpatient radiology network boosted document processing capacity by 50%, allowing specialists to handle 130–150 documents daily instead of 100. This efficiency equated to the workload of 30+ full-time employees.
Metric | Before Real-Time Monitoring | After Real-Time Monitoring | Improvement |
|---|---|---|---|
Patient Wait Time (Dermatology) | 22 minutes | 4 minutes | 82% reduction |
Data Entry Time (Dermatology) | 2–3 hours/day | 15 minutes/day | 92% reduction |
Median Cycle Time (MD Anderson) | 91 minutes | 72 minutes | 21% reduction |
Cumulative Wait Time (MD Anderson) | 45 minutes | 16 minutes | 64% reduction |
Staff Travel Time (Oregon Medical) | Baseline | 90 min saved/day | 90 min saved |
These advancements also expand clinical capacity. For instance, MD Anderson's reduced cycle times allowed them to see more patients without extending work hours. Faster pre-visit workflows mean clinics can accommodate higher patient volumes while maintaining high-quality care - an essential advantage when new patient appointment wait times in large metropolitan areas reached 31 days in 2025.
How to Implement Real-Time Monitoring in Clinics
Clinics can achieve substantial efficiency improvements by methodically introducing real-time monitoring systems. This requires focusing on three main areas: technical integration, security compliance, and staff training.
System Integration and Workflow Customization
Before diving into new technology, it’s critical to map out existing workflows. For example, MD Anderson’s Patient Flow Analysis (Feb 2019–Sep 2020) reviewed 556 consults and revealed inefficiencies like redundant tasks and unclear responsibilities. By identifying these bottlenecks, they were able to make precise adjustments.
For seamless technical integration, use standard APIs like HL7 Fast Healthcare Interoperability Resources (FHIR) to link monitoring tools with systems such as EMRs or Radiology Information Systems. If your clinic is transitioning from analog systems, middleware can act as a bridge. A great example comes from Amplify Care, which used a Business Automation Workflow (BAW) platform between May 2022 and December 2023 to connect digital eReferral systems with fax-dependent providers. This approach processed 4,504 eFaxes for 4,132 patients, and after introducing automated retry logic in March 2023, fax failure rates dropped from 37.7% to 9.9%.
Workflow customization is equally important. MD Anderson adjusted staff roles so medical assistants handled rooming tasks, allowing registered nurses to focus on patient education. This reduced visit times over two hours from 22% to 0%. A 10–14-day pilot program can help refine these changes before a full rollout.
Once the technical groundwork is in place, the next step is ensuring robust data security and compliance.
Compliance and Data Security
Before launching any system, conduct Privacy Impact Assessments (PIA) and Threat Risk Assessments (TRA) to uncover vulnerabilities. Patient data must be encrypted using AES-256 for storage and TLS 1.3 during transmission. Additionally, automatic detection of Protected Health Information (PHI) is essential to prevent sensitive data from being logged into non-compliant systems.
It’s also crucial to execute Business Associate Agreements (BAA) with every technology vendor involved. For example, implementing an AI-powered intake system could cost around $7,500 for initial setup, with ongoing expenses of about $450 per month for maintaining HIPAA-compliant databases, SMS services, and AI API calls. These measures ensure patient data integrity, creating a smoother experience for both staff and patients.
Staff Training and Change Management
Getting staff on board is vital. At MD Anderson, nursing staff, physicians, IT teams, and administrators were involved early in the planning process, which helped reduce resistance and build enthusiasm for the changes. Assigning physician champions can also help refine workflow templates.
Training is often straightforward. For example, staff at MD Anderson quickly learned to use the Patient Status function in their Epic EMR for real-time updates, which eliminated unnecessary back-and-forth communication. Training sessions should focus on practical features like status boards and communication tools to ensure a smooth transition.
Addressing resistance to new technology is another key factor. In Ontario, 88% of physicians were still using fax machines as of 2021, demonstrating the challenge of moving away from older methods. Amplify Care tackled this by offering solutions that worked for both digital adopters and those still reliant on fax systems, minimizing disruption.
Conclusion
Real-time monitoring shifts outdated, reactive workflows into streamlined, proactive processes. With automated onboarding, practices can reduce timelines from two weeks to same-day completion. These advancements completely overhaul administrative tasks, making them more efficient and less time-consuming.
Take, for instance, a dermatology practice that invested $12,900 and saw an annual return of $185,000 - a staggering 1,334% ROI. This freed up staff from tedious data entry, allowing them to focus on what matters most: patient care. Gabriela Castro from Always Keep Progressing shared her experience:
"Before Solum, it was almost a full day on the phone. Now we have more time to focus on other things. Definitely it's been so helpful."
These changes go beyond immediate cost savings. With patient visits expected to grow by 16% over the next decade, clinics adopting real-time monitoring can handle increased demand without adding more administrative burden. This technology not only supports scalability but also enhances care quality and boosts patient satisfaction.
FAQs
What is real-time monitoring in pre-visit workflows?
Real-time monitoring in pre-visit workflows revolves around tracking patient data and responses as they come in, allowing clinics to address concerns right away. For example, AI systems can instantly validate patient forms or reminders, ensuring everything is accurate and up to date. Additionally, real-time location tracking helps optimize scheduling and cut down on wait times. The result? Smoother operations, better accuracy, and a more seamless experience for patients before their appointments.
How long does it take to implement real-time monitoring in a clinic?
Implementing real-time monitoring in a clinic usually takes around 14 days. For instance, a dermatology practice managed to integrate AI-powered intake systems within this period by following a streamlined audit-to-action process. However, the exact timeline can differ based on the clinic's unique requirements and current workflows.
How do clinics keep patient data HIPAA-compliant with these tools?
Clinics ensure HIPAA compliance through a combination of rigorous practices. They enforce strict security policies, rely on secure systems for managing sensitive data, and use tools that work effortlessly with electronic health records (EHRs). These steps are crucial for safeguarding patient confidentiality and maintaining the accuracy of healthcare data.
Related Blog Posts
Real-time monitoring is transforming how clinics handle pre-visit workflows, cutting down inefficiencies and improving patient care. It reduces wait times, minimizes errors, and saves staff hours by automating tasks like data entry and insurance verification. For example, clinics using AI-powered systems have seen patient wait times drop by 82% and data entry errors reduced to 0.3%. These tools also streamline processes, allowing clinics to handle more patients without overburdening staff.
Key benefits include:
Time savings: Clinics save hours daily by automating manual tasks.
Improved accuracy: Data entry error rates drop significantly.
Shorter wait times: Patients experience faster service, enhancing satisfaction.
Higher ROI: Some clinics report over 1,300% return on investment.
Research Findings: Real-Time Monitoring Benefits for Pre-Visit Workflows
Time Savings and Efficiency Improvements
Real-time monitoring systems have made a noticeable impact on clinic operations, especially in terms of time management and efficiency. For example, the University of Michigan Kellogg Eye Center implemented a passive RFID real-time locating system in their glaucoma clinic between January and July 2018. Across 1,972 patient visits, the system shaved 2.9 minutes off technician process times per patient, saving around 156 minutes daily. This efficiency boost allowed the clinic to increase its daily patient load from 51.9 to 58.4, all without extending overall wait times.
Similarly, MD Anderson Cancer Center's Department of Gastrointestinal Radiation Oncology adopted real-time EMR tracking for 556 consultation visits between May 2019 and September 2020. This initiative reduced the median cycle time by 21%, cutting it from 91 minutes to 72 minutes. Cumulative waiting times dropped by 64%, going from 45 minutes to just 16 minutes. Additionally, the proportion of visits exceeding two hours fell from 22% to 0%.
These improvements highlight how real-time monitoring not only saves time but also enhances the overall efficiency of pre-visit workflows.
Better Data Accuracy and Workflow Reliability
Accurate data is crucial in creating reliable workflows, and real-time systems have delivered impressive results. A dermatology practice operating across three offices introduced a HIPAA-compliant AI intake system to process over 300 forms weekly. Within just 30 days, this system reduced data entry error rates from 3.8% to 0.3%, improved pre-visit insurance verification rates from 0% to 94%, and cut manual data entry time from 2–3 hours per day to just 15 minutes. The system utilized OCR and a natural language processing engine tailored for medical terminology, ensuring any low-confidence data entries were flagged for staff review.
In another example, Amplify Care in Ontario implemented a Business Automation Workflow platform to streamline e-Referrals and fax systems. By adding automated retry logic in March 2023, they reduced fax failure rates from 37.7% to 9.9%, achieving a 98.7% successful delivery rate across 4,504 e-Faxes for 4,132 patients.
These advancements in data accuracy not only minimize errors but also reduce delays, making pre-visit processes more dependable.
Fewer Pre-Visit Delays
Real-time monitoring has also proven effective in cutting down pre-visit delays. The dermatology practice mentioned earlier achieved an 82% reduction in patient wait times, bringing the average wait from 22 minutes to just 4 minutes. This was accomplished by completing data entry and insurance verification ahead of time using digital intake links sent to patients 48 hours before their appointments.
In radiation oncology, real-time EMR status boards improved communication among nursing staff, residents, and attending physicians. By clarifying roles and eliminating redundant tasks like repeated history-taking, these systems helped streamline the workflow from registration to consultation.
Technologies That Enable Real-Time Monitoring
AI-Powered Document Management
AI has transformed document management by automating processes like fax triage and referral tracking. Using OCR (Optical Character Recognition) and NLP (Natural Language Processing), these systems extract data from handwritten forms, insurance cards, and faxes with accuracy rates reaching up to 99.2%.
Take Penn Medicine, for example. In November 2025, they rolled out "coordn8", an AI-driven system designed for fax processing and digital consent. This tool processed 3,000 faxes daily, saving 8,500 staff hours over 18 months. It also slashed the time needed to obtain patient signatures by 85% through text-based eDisclosure. Jency Daniel highlighted the impact:
"Reducing processing time allows staff to focus on more patient-facing activities and results in higher job satisfaction. Vacations or sick days won't slow the process down anymore."
A similar success story unfolded in January 2026 when a major U.S. health insurer partnered with Alithya. By applying Small Language Models, they automated 97% of fax submissions, achieved 80% straight-through processing, and saved $2.2 million annually.
Platforms like Diagna's FAXFlo bring these capabilities to specialty clinics. FAXFlo automatically receives, reads, categorizes, and routes incoming faxes. It also extracts key patient details, links documents to the correct EMR record, and saves over four hours of staff time daily with over 98% accuracy.
These AI-powered tools lay the groundwork for further automation, including scheduling and seamless EMR integration.
Automated Scheduling and Reminders
While AI streamlines document handling, automated scheduling tools improve patient readiness and reduce no-shows. Digital intake engines send secure links to patients, allowing them to complete demographics, verify insurance, and answer condition-specific questions from the comfort of their homes. Responses sync directly with the EHR, and research shows that 77% of patients prefer this digital approach for completing pre-visit forms.
Real-time wait tracking systems take patient convenience a step further. By providing updates on queue positions and predicting wait times with over 94% accuracy via SMS, these platforms ease patient anxiety and reduce walk-outs. They can also send apology messages for delays and follow-up reminders based on diagnoses. With no app downloads required, SMS-based systems have adoption rates exceeding 60%.
Additionally, automated systems save staff time by handling routine tasks like notifying patients of lab results and managing callbacks, freeing up around 10 hours per week.
EMR Integration
Once data is captured and appointments are scheduled, EMR integration ensures everything flows smoothly into patient care. Modern systems use HL7 FHIR standards and APIs to securely synchronize data.
This two-way synchronization means information from digital forms, insurance verifications, and referrals automatically updates in the EMR. Staff no longer need to re-enter data, which ensures patient charts are complete and ready when the visit begins. As Solum Health explains:
"Clean data posts to the EHR and the scheduling and billing queues through API integration. On arrival, the chart is complete, the front desk sees what is pending, and the visit starts on time."
Between May 2022 and December 2023, Amplify Care tested a system in Ontario that integrated an eReferral platform with fax-reliant receivers using HL7 FHIR. The platform processed 4,504 eFaxes for 4,132 unique patients. By March 2023, new retry logic reduced fax failure rates from 37.7% to 9.9%, with 98.7% of eFaxes successfully delivered after retries.
Diagna offers EMR integration that works with any system, allowing clinics to maintain their current workflows. This flexibility ensures that automated document processing and referral tracking integrate seamlessly, delivering real-time updates and fully completed charts without disrupting existing processes.
Making Clinical AI Work: Workflow-Native Automation and the Future of Healthcare Efficiency
Clinical and Operational Results from Real-Time Monitoring

Real-Time Monitoring Impact on Clinical Workflows: Before vs After Results
The efficiency gains from real-time monitoring are making a noticeable difference in healthcare, improving both operations and clinical outcomes across various settings.
Staff Time Savings and Increased Productivity
Real-time monitoring is reshaping how clinics operate. For instance, Oregon Medical Group implemented a Real-Time Location System (RTLS) that allowed patients to self-room after registration. This eliminated the need for staff to shuttle patients between waiting areas and exam rooms. Steve Liu, their Director of IT, shared:
"The efficiencies we've gained from using CenTrak's RTLS system have been quite incredible. Patients are getting more time with their care team while also experiencing a decrease in appointment wait times."
Another example comes from a dermatology practice with eight providers across three locations. By automating data entry, they slashed the time spent on this task by 92%, going from 2–3 hours daily to just 15 minutes per location. The practice administrator highlighted the financial impact:
"Our front desk staff were spending half their day typing data from forms into Athenahealth. Now the AI handles it before the patient even walks in. The $7,500 investment paid for itself in the first month."
At MD Anderson Cancer Center, the Department of Gastrointestinal Radiation Oncology saw impressive results from using real-time tracking in their Epic EMR. This system eliminated duplicate tasks and clarified nursing roles for 556 consults between 2019 and 2020. As a result, visits lasting over two hours dropped from 22% to 0%, significantly cutting cycle times and patient waiting periods.
These changes free up staff to focus on what really matters - patient care - while making the overall experience more seamless.
Better Patient Satisfaction and Care Quality
Improved workflows and shorter wait times are directly enhancing patient satisfaction. The dermatology practice mentioned earlier saw its Google review rating rise from 4.1 to 4.6 stars, while negative comments about wait times dropped by 78%. This was largely due to the reduction in patient wait times to just four minutes.
Another success story comes from the pediatric therapy clinic Always Keep Progressing, which reduced its patient onboarding process by 99% - from two weeks to same-day completion. Gabriela Castro, the Clinic Manager, explained how this change has positively impacted their operations:
"Before Solum, it was almost a full day on the phone. Now we have more time to focus on other things. Definitely it's been so helpful."
Patients also appreciated the simpler process. Castro added:
"The feedback from the patients is like kind of easier for them. Just with that link, and then if they have any question they can just ask for an in-person representative."
Additionally, the clinic automated all insurance verifications, eliminating last-minute surprises and reducing the need to reschedule due to coverage issues.
These operational upgrades not only enhance care but also lead to financial rewards.
Financial Impact and ROI
The financial benefits of real-time monitoring are undeniable. For example, the dermatology practice invested $12,900 in the first year and generated a $185,000 annual impact, achieving an ROI of 1,334%. They also reduced data entry error rates from 3.8% to 0.3%.
On a larger scale, Atrium Health Wake Forest reported a $10 million total benefit from Enterprise Location Services, while Piedmont Healthcare saved $500,000 annually by standardizing asset management and cutting rental and maintenance costs. Meanwhile, an outpatient radiology network boosted document processing capacity by 50%, allowing specialists to handle 130–150 documents daily instead of 100. This efficiency equated to the workload of 30+ full-time employees.
Metric | Before Real-Time Monitoring | After Real-Time Monitoring | Improvement |
|---|---|---|---|
Patient Wait Time (Dermatology) | 22 minutes | 4 minutes | 82% reduction |
Data Entry Time (Dermatology) | 2–3 hours/day | 15 minutes/day | 92% reduction |
Median Cycle Time (MD Anderson) | 91 minutes | 72 minutes | 21% reduction |
Cumulative Wait Time (MD Anderson) | 45 minutes | 16 minutes | 64% reduction |
Staff Travel Time (Oregon Medical) | Baseline | 90 min saved/day | 90 min saved |
These advancements also expand clinical capacity. For instance, MD Anderson's reduced cycle times allowed them to see more patients without extending work hours. Faster pre-visit workflows mean clinics can accommodate higher patient volumes while maintaining high-quality care - an essential advantage when new patient appointment wait times in large metropolitan areas reached 31 days in 2025.
How to Implement Real-Time Monitoring in Clinics
Clinics can achieve substantial efficiency improvements by methodically introducing real-time monitoring systems. This requires focusing on three main areas: technical integration, security compliance, and staff training.
System Integration and Workflow Customization
Before diving into new technology, it’s critical to map out existing workflows. For example, MD Anderson’s Patient Flow Analysis (Feb 2019–Sep 2020) reviewed 556 consults and revealed inefficiencies like redundant tasks and unclear responsibilities. By identifying these bottlenecks, they were able to make precise adjustments.
For seamless technical integration, use standard APIs like HL7 Fast Healthcare Interoperability Resources (FHIR) to link monitoring tools with systems such as EMRs or Radiology Information Systems. If your clinic is transitioning from analog systems, middleware can act as a bridge. A great example comes from Amplify Care, which used a Business Automation Workflow (BAW) platform between May 2022 and December 2023 to connect digital eReferral systems with fax-dependent providers. This approach processed 4,504 eFaxes for 4,132 patients, and after introducing automated retry logic in March 2023, fax failure rates dropped from 37.7% to 9.9%.
Workflow customization is equally important. MD Anderson adjusted staff roles so medical assistants handled rooming tasks, allowing registered nurses to focus on patient education. This reduced visit times over two hours from 22% to 0%. A 10–14-day pilot program can help refine these changes before a full rollout.
Once the technical groundwork is in place, the next step is ensuring robust data security and compliance.
Compliance and Data Security
Before launching any system, conduct Privacy Impact Assessments (PIA) and Threat Risk Assessments (TRA) to uncover vulnerabilities. Patient data must be encrypted using AES-256 for storage and TLS 1.3 during transmission. Additionally, automatic detection of Protected Health Information (PHI) is essential to prevent sensitive data from being logged into non-compliant systems.
It’s also crucial to execute Business Associate Agreements (BAA) with every technology vendor involved. For example, implementing an AI-powered intake system could cost around $7,500 for initial setup, with ongoing expenses of about $450 per month for maintaining HIPAA-compliant databases, SMS services, and AI API calls. These measures ensure patient data integrity, creating a smoother experience for both staff and patients.
Staff Training and Change Management
Getting staff on board is vital. At MD Anderson, nursing staff, physicians, IT teams, and administrators were involved early in the planning process, which helped reduce resistance and build enthusiasm for the changes. Assigning physician champions can also help refine workflow templates.
Training is often straightforward. For example, staff at MD Anderson quickly learned to use the Patient Status function in their Epic EMR for real-time updates, which eliminated unnecessary back-and-forth communication. Training sessions should focus on practical features like status boards and communication tools to ensure a smooth transition.
Addressing resistance to new technology is another key factor. In Ontario, 88% of physicians were still using fax machines as of 2021, demonstrating the challenge of moving away from older methods. Amplify Care tackled this by offering solutions that worked for both digital adopters and those still reliant on fax systems, minimizing disruption.
Conclusion
Real-time monitoring shifts outdated, reactive workflows into streamlined, proactive processes. With automated onboarding, practices can reduce timelines from two weeks to same-day completion. These advancements completely overhaul administrative tasks, making them more efficient and less time-consuming.
Take, for instance, a dermatology practice that invested $12,900 and saw an annual return of $185,000 - a staggering 1,334% ROI. This freed up staff from tedious data entry, allowing them to focus on what matters most: patient care. Gabriela Castro from Always Keep Progressing shared her experience:
"Before Solum, it was almost a full day on the phone. Now we have more time to focus on other things. Definitely it's been so helpful."
These changes go beyond immediate cost savings. With patient visits expected to grow by 16% over the next decade, clinics adopting real-time monitoring can handle increased demand without adding more administrative burden. This technology not only supports scalability but also enhances care quality and boosts patient satisfaction.
FAQs
What is real-time monitoring in pre-visit workflows?
Real-time monitoring in pre-visit workflows revolves around tracking patient data and responses as they come in, allowing clinics to address concerns right away. For example, AI systems can instantly validate patient forms or reminders, ensuring everything is accurate and up to date. Additionally, real-time location tracking helps optimize scheduling and cut down on wait times. The result? Smoother operations, better accuracy, and a more seamless experience for patients before their appointments.
How long does it take to implement real-time monitoring in a clinic?
Implementing real-time monitoring in a clinic usually takes around 14 days. For instance, a dermatology practice managed to integrate AI-powered intake systems within this period by following a streamlined audit-to-action process. However, the exact timeline can differ based on the clinic's unique requirements and current workflows.
How do clinics keep patient data HIPAA-compliant with these tools?
Clinics ensure HIPAA compliance through a combination of rigorous practices. They enforce strict security policies, rely on secure systems for managing sensitive data, and use tools that work effortlessly with electronic health records (EHRs). These steps are crucial for safeguarding patient confidentiality and maintaining the accuracy of healthcare data.