How Clinics Overcome AI Adoption Challenges
Healthcare Technology
Healthcare Technology
Guide for clinics to assess AI readiness, build governance, and run low-risk pilots (fax triage, referrals, prior auth) to reduce admin time and costs.
Guide for clinics to assess AI readiness, build governance, and run low-risk pilots (fax triage, referrals, prior auth) to reduce admin time and costs.

AI is transforming outpatient clinics by automating tedious tasks like scheduling, fax sorting, and prior authorizations. While 71% of U.S. hospitals used AI in electronic health records by 2024, many clinics face hurdles like high costs, compliance concerns, and staff training gaps. This guide explains how clinics can prepare for AI, tackle barriers, and measure success with low-risk pilots in areas like document handling.
Key Takeaways:
Challenges: Financial concerns (47% cite unclear ROI), compliance issues (40% worry about HIPAA), and integration problems (77% struggle with legacy systems).
Solutions: Conduct readiness assessments, prioritize barriers, and start with manageable AI projects (e.g., automating fax triage).
Results: AI can cut administrative costs by 10–20% and save clinicians 3 hours weekly by reducing after-hours documentation.
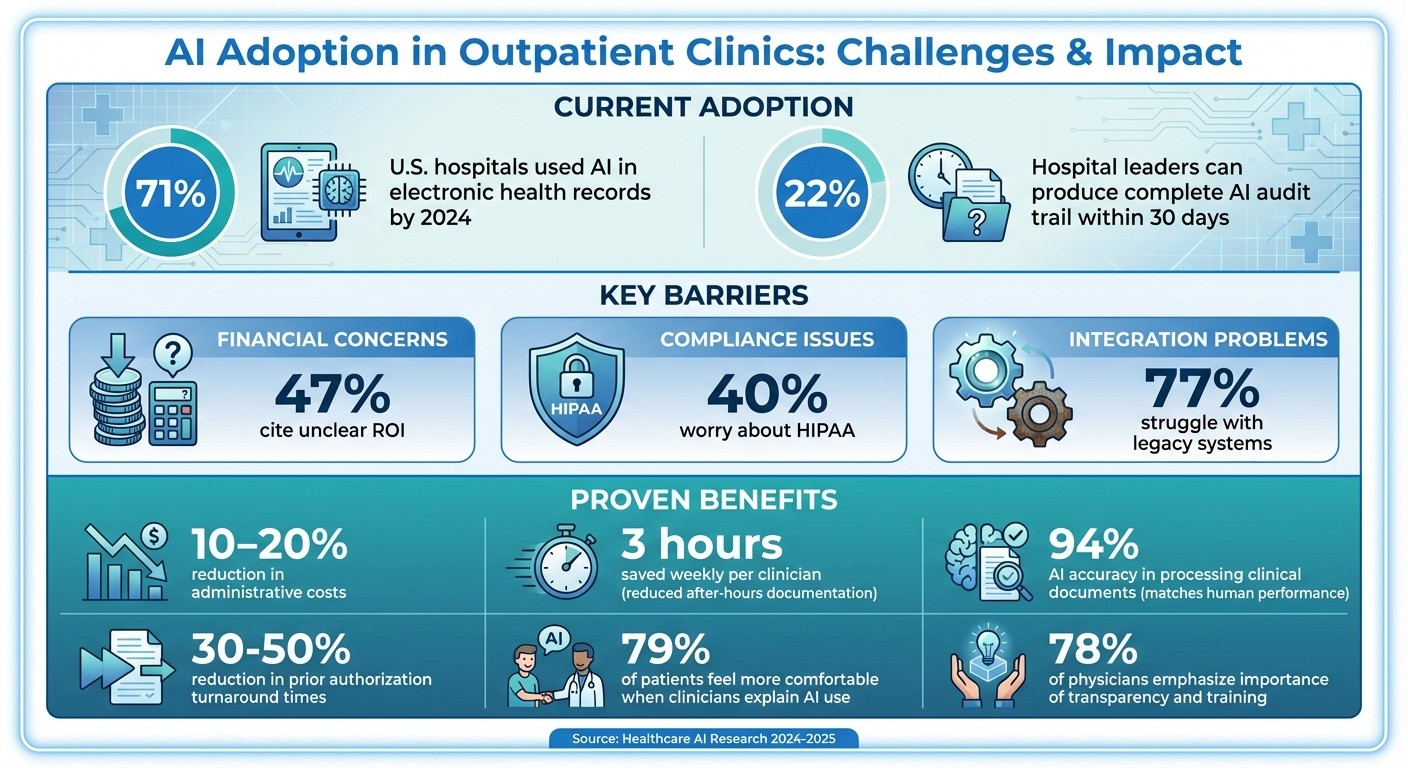
AI Adoption Challenges and Benefits in Healthcare Clinics
AI in Healthcare 2025: November Breakthroughs for Your Practice
Evaluating Your Clinic's Readiness for AI
Before diving into AI adoption, it's essential to take stock of your clinic's current capabilities. A structured readiness assessment can provide a clear view of your strengths and weaknesses, helping you pinpoint areas that need attention. This evaluation lays the groundwork for the adjustments needed to ensure a smooth AI implementation.
Running a Readiness Assessment
To address the challenges of integrating AI, start by evaluating six key areas: EMR/EHR capabilities, data quality, people and skills, workflows and processes, technology infrastructure, and governance and compliance. For example, check if your EMR system supports APIs like HL7/FHIR and whether it can automatically update patient records.
Assess the quality of your data, focusing on areas like patient demographics, problem lists, and insurance details. Are referrals and prior authorizations arriving as structured, usable data, or are they messy faxes requiring manual intervention? Poor data quality is a common roadblock when rolling out AI solutions.
Next, evaluate your team's comfort level with digital tools such as patient portals or e-prescribing systems. Identifying a "clinical champion" to lead the way in piloting new workflows can be a game-changer, especially for smaller outpatient clinics that may lack specialized IT staff or robust training programs.
Your technology infrastructure is another critical area. Do you have secure internet connectivity, enough devices, and the capacity to support cloud-based tools while staying compliant with HIPAA requirements? Lastly, review your governance processes - whether formal or informal - for approving, monitoring, and auditing digital tools. A 2025 Black Book Research survey revealed that only 22% of hospital leaders could produce a complete AI audit trail within 30 days, showing that oversight gaps are still a major issue.
To simplify this process, create a checklist and score your clinic on a scale of 1 to 5 across these areas. This will give you a baseline readiness score and help identify where to invest before launching AI initiatives.
Mapping and Prioritizing Your Barriers
Once you've completed your readiness assessment, it’s time to map out the specific challenges your clinic faces. Organize a workshop with practice leaders, clinicians, front-office staff, and billing teams to identify perceived barriers. These challenges often fall into four categories:
Financial: Concerns over ROI, upfront costs, and subscription fees.
Technical: Limited EHR integration, poor data quality, or weak connectivity.
Workflow: Disruptions to existing processes and unclear task ownership.
Cultural: Fears about errors, liability, job security, or resistance to change.
Financial concerns often top the list, with unclear ROI and ongoing costs being major sticking points. Addressing these requires seamless integration into current workflows, transparency, and thorough training to build trust in AI tools.
Document these barriers using a spreadsheet or whiteboard, then prioritize them using a simple 2×2 grid. This grid compares the impact of each barrier on clinical or operational goals with the urgency of addressing it. High-impact, high-urgency issues - like revenue loss from delayed referrals or severe staff shortages - should take precedence. Lower-impact concerns, like minor interface glitches, can be addressed later. For many outpatient clinics, the most common challenges are workflow integration, data and infrastructure gaps, and financial uncertainty. Developing a focused action plan, such as standardizing referral intake processes or clarifying AI budgets with expected savings, can help tackle these issues before moving forward with a pilot.
Once you've identified and prioritized your barriers, set clear metrics to measure your progress.
Setting Measurable Success Metrics
Before rolling out any AI tool, establish baseline metrics that reflect both operational efficiency and financial performance. These metrics should address the financial, technical, and workflow challenges identified earlier. Consider tracking:
Average time from fax receipt to EMR indexing
Percentage of misfiled or lost faxes
Average referral processing time
Turnaround time for prior authorization requests
Total staff hours spent weekly on pre-visit administrative tasks
Additionally, monitor staff overtime related to administrative tasks, costs for temporary staff during peak periods, rates of denied or delayed claims due to missing documentation, and revenue losses from incomplete referrals.
Research shows that AI, when deployed effectively, can cut hospital operating costs by 10–20%, largely through administrative efficiencies. Setting SMART (Specific, Measurable, Achievable, Relevant, Time-bound) goals ensures you can track progress objectively. For instance, you might aim to reduce weekly staff hours spent on fax triage and indexing by 30% within six months of implementing AI, or cut referral processing times from five days to two. Similarly, you could target a 50% reduction in prior authorization turnaround times and a 40% drop in claims denials caused by missing documentation.
For pre-visit workflows, platforms like Diagna offer automation tools for fax triage, referral tracking, and prior authorization processing while integrating seamlessly with any EMR. As part of your readiness evaluation, review your current document volume, error rates in manual indexing, and the frequency of delays caused by incomplete referrals or authorizations. These baseline measurements will help you set realistic goals and demonstrate the ROI of your AI solution once it's live.
Establishing Governance, Compliance, and Trust
Once you've assessed your readiness and identified potential obstacles, the next step is to establish a strong governance framework that ensures your AI tools are safe, compliant, and trusted by your team. This structure connects your earlier evaluations to practical implementation, making sure AI is deployed responsibly and effectively.
Creating an AI Governance Framework
For an outpatient clinic, an effective governance framework typically focuses on five key areas: strategy and use-case selection, risk and safety oversight, data and privacy management, IT/security and integration, and training and change management. Assigning specific responsibilities to designated leads is essential.
Strategy and Use-Case Selection: A clinical or medical director, along with an operations leader, should handle strategy. Their role is to identify AI tools that align with the clinic's goals, whether it's improving patient access, enhancing care quality, or boosting revenue.
Risk and Safety Oversight: A clinician champion and a quality or safety representative should define what "safe use" looks like within your workflows. For example, staff should review all AI-generated document classifications before appointments or orders are triggered.
Data and Privacy Management: A compliance or privacy officer ensures HIPAA-compliant data handling, secures Business Associate Agreements (BAAs), and maintains audit trails for any AI tools interacting with protected health information.
IT/Security and Integration: An IT lead should evaluate vendors for security measures, system uptime, and electronic medical record (EMR) compatibility. They should also track model versions and system interfaces for audit purposes.
Training and Change Management: Clinical leadership and HR or education coordinators should provide role-specific training, outline approved workflows, and reinforce the importance of "human in the loop" oversight.
Clearly defining human responsibilities for each workflow step is critical. For instance, while AI-powered fax triage can classify and extract data, a referral coordinator should verify the classifications and key fields before creating orders. Specify which decisions AI can handle independently (e.g., assigning a fax to a "referrals" queue), which require human review (e.g., verifying provider details), and which are strictly reserved for clinicians (e.g., modifying a care plan). Many clinics streamline this process through an AI steering group that meets monthly to review proposals, monitor performance metrics, and approve changes before scaling.
Meeting Regulatory and Privacy Requirements
When implementing AI in pre-visit workflows, compliance with U.S. regulations like HIPAA, FTC and state consumer protection laws, and FDA guidance on software as a medical device (SaMD) is crucial. HIPAA governs the handling of protected health information (PHI), so any AI interacting with patient data must operate under a HIPAA-compliant framework with proper safeguards, access controls, and data minimization practices.
Administrative tools like fax classification generally fall outside FDA SaMD criteria since they don't provide diagnostic recommendations. However, ensure vendors position their software as operational support rather than clinical decision-making tools. The FDA's evolving guidance on AI/ML-enabled medical software applies if a tool influences clinical decisions or risk scores.
To maintain compliance, create a HIPAA checklist covering:
Legal Agreements: Secure a signed BAA outlining permitted PHI uses, breach notification timelines, subcontractor obligations, and data return or destruction policies.
Data Handling: Limit PHI usage to agreed purposes, with clear policies on retention, deletion, and disclosure during model training.
Security Controls: Implement encryption (in transit and at rest), role-based access controls, regular penetration testing, and incident response plans. Request third-party security certifications or audits.
Transparency and Logging: Maintain detailed logs of system access, model versions, configuration changes, and key automated actions to ensure auditability.
When evaluating vendors, use a standardized questionnaire to assess regulatory compliance, privacy protections, security measures, and operational fit. Key questions include whether the software qualifies as SaMD, what PHI it processes, whether data leaves the U.S., and how data minimization is handled. Request documentation on encryption standards, access controls, vulnerability management, and independent security assessments. For tools like Diagna's fax triage and prior authorization automation, confirm the platform operates under a BAA, integrates securely with your EMR, and provides exportable logs and admin dashboards for audits.
Building Staff and Clinician Confidence
Even the most robust governance framework won't succeed if your team doesn't trust the technology. Building confidence among clinicians and staff requires transparent communication, targeted training, and sharing validation data. A 2023 survey revealed that 78% of physicians emphasized the importance of transparency and training when using health AI, while 79% of patients reported feeling more comfortable when clinicians explained AI use.
Explain what the AI does, what it doesn't do, and where human oversight remains essential. For example, while AI may classify documents and extract data, a staff member should always verify these outputs before taking further action. Share validation data and real-world results - such as accuracy rates, time saved, and error reductions - to demonstrate the tool's benefits and limitations.
"Our software is built keeping in all regulatory guidelines from HIPAA. We base our workflows on top industry guidelines ensuring no compromise to data safety." – Diagna.ai
Involve clinicians during both design and implementation to ensure the tools meet practical needs. Focus on creating user-friendly interfaces that integrate seamlessly with EMR workflows, allowing data to sync directly into patient charts without manual effort. Starting with repetitive, high-volume tasks like fax triage, email sorting, and prior authorization form filling can help ease the transition. As staff see the AI delivering accurate results and saving significant time - potentially over 20 hours per week - they'll likely feel more comfortable expanding its use. Regularly reviewing performance dashboards to track usage, error rates, and any incidents ensures you can address concerns quickly and maintain trust.
Starting with High-Value, Low-Risk AI Solutions
Once you’ve established a strong governance framework, the next logical step is to kick off low-risk AI projects. The best starting point? Focus on administrative and pre-visit workflows that save time without impacting clinical decisions. Tasks like document handling, referral tracking, and prior authorization fit the bill perfectly. These processes are high-volume, follow clear rules, and take up a lot of staff time, but they carry minimal clinical risk when managed with proper oversight.
Automating Pre-Visit Workflows with AI
Using your governance framework as a foundation, start automating repetitive pre-visit tasks. U.S. clinics often see great results from three specific workflows: document triage, referral tracking, and prior authorization automation. Here's how each works:
Document triage: AI tools classify and extract critical data from faxes, such as lab results or referrals, and route them to the right folders in the EMR. This cuts sorting time in half and reduces routing errors.
Referral tracking: AI centralizes incoming referrals, tracks which patients have scheduled appointments, and flags those who haven’t, improving access and capturing revenue.
Prior authorization automation: AI pre-fills payer-specific forms using chart data, checks for missing details, and tracks submission progress, reducing turnaround times by 30–50%.
Diagna's tools - FAXFlo, Referral Manager, and Prior Auth Bot - integrate directly with your EMR, pushing structured data into the right fields and queues. This eliminates the need for staff to retype information or toggle between systems. AI accuracy in processing clinical documents has reached 94%, matching human performance and ensuring same-day document handling.
"Our AI integrates around your workflows, not the other way around - no matter which EMR you use." – Diagna.ai
Testing AI with Small-Scale Pilots
A smart way to introduce AI is through small, controlled pilots. Begin by defining clear boundaries: choose a single workflow (like handling inbound referral faxes), limit it to one department, and run it for 60–90 days with a manageable volume, such as up to 200 faxes daily. Before starting, collect baseline data, including processing time per item, staff hours spent, error rates, and the time from referral receipt to appointment scheduling. Identify potential issues, like misrouted faxes or missed referrals, and establish clear escalation procedures.
Provide brief training sessions and simple guides to help staff understand how to use the AI and handle exceptions. Assign specific clinical or operational owners, as well as IT/data leads, to oversee the process and address any issues like misclassifications or downtime. Hold weekly reviews to analyze data, gather feedback, and make necessary adjustments. At the end of the pilot, compare the results to your baseline, evaluate staff feedback, and decide whether to stop, extend, or expand the project. If the pilot meets success criteria, you can scale the solution to other workflows.
Connecting AI with Your EMR System
For AI to be effective, it needs to work seamlessly with your EMR. This means AI outputs should appear in the same screens and queues your staff already use, avoiding the need for separate portals that create extra work. Collaborate with your vendor and EMR team to use existing interfaces and APIs - like HL7 or FHIR - to ensure AI outputs are stored as structured data, correctly linked to the right patient and provider. Route AI-generated tasks to established work queues (e.g., "referral work queue" or "prior auth work queue") so staff can manage them within familiar workflows.
To enhance tracking and quality oversight, configure specific fields populated by AI - such as referral reasons, referring providers, payers, and authorization IDs. These fields should be searchable and reportable. Before going live, test the integration in a controlled environment to ensure proper patient matching, document routing, and user permissions.
Training Staff and Scaling AI Adoption
Providing Role-Specific AI Training
To successfully integrate AI tools into healthcare workflows, it's crucial to provide tailored training for each role. Front-desk staff, clinicians, and billing coordinators all interact with AI differently, so their training should reflect these unique needs. For instance, front-desk and access teams need hands-on experience with AI tools for scheduling, patient intake, and insurance verification. Clinicians must focus on interpreting AI outputs, understanding its limitations (like occasional inaccuracies), and maintaining clinical judgment to avoid over-reliance on automation. Billing coordinators, on the other hand, should master AI features like claim scrubbing, coding suggestions, and automated prior authorization workflows, with a strong emphasis on compliance and escalation procedures.
A tiered micro-learning approach works well here. Start with 20–30 minute onboarding sessions tailored to each role, followed by short refresher modules every three to six months. Use a mix of formats, such as live demonstrations within the EMR, quick e-learning modules, and job aids integrated into daily workflows. To minimize disruptions, schedule these sessions during protected times like monthly staff meetings or quick team huddles. Designating "AI super-users" in each role can also provide just-in-time peer support and coaching.
Training must also address key concerns like safety, privacy, and the scope of AI use. Staff should understand how patient data is protected, what information is shared with vendors, and how AI outputs are monitored. Hands-on exercises - like comparing manual referral triage with AI-driven automation - can help staff see the practical benefits, such as time savings, while reinforcing that final decisions remain human-led. A Philips survey revealed that 79% of patients felt more comfortable when clinicians clearly explained how AI was being used. Leaders should emphasize that AI is designed to reduce administrative burdens, not replace staff, which can help lower burnout and improve job satisfaction.
Updating Policies and Workflows
Effective AI adoption requires updated policies and workflows that align with new practices. Start by clearly defining approved AI use cases, mandatory human reviews, and role-based responsibilities. Document how AI outputs will integrate into the EMR, specifying where AI-generated notes or triaged documents will appear, how they’ll be labeled, and the escalation process for discrepancies. Establish robust audit and logging practices - an area where only about 22% of hospitals currently feel confident.
Job descriptions should also be updated to include expectations around AI tool usage, performance monitoring, and ongoing training participation. Collaborate with vendors and IT teams to ensure AI tools seamlessly integrate with existing systems, like EMRs and task queues. For example, AI-based fax management should route triaged documents directly into the same EMR work queues staff already use, eliminating the need for multiple logins or duplicate data entry. Poorly integrated tools can disrupt workflows and lead to inefficiencies, even when the AI itself performs accurately.
Tracking Performance and Expanding Use Cases
Once staff are trained and workflows are updated, ongoing performance tracking becomes essential. Monitoring key performance indicators (KPIs) helps ensure AI adoption improves efficiency without compromising patient care. Focus on metrics like referral-to-appointment times, the speed of fax/referral processing (e.g., percentage completed within 24–48 hours), prior authorization turnaround times, denied claims reduction, and staff overtime costs. Studies suggest well-implemented AI can cut hospital operating costs by 10–20%. Additionally, track experiential metrics like staff satisfaction, burnout levels, appointment wait times, and call-back speeds. Establish baseline metrics before AI implementation and review them regularly - such as 60 to 90 days post-launch - to identify areas needing further training or adjustments.
To refine processes, create structured feedback loops. Use tools like brief pulse surveys, periodic focus groups, or an EMR-embedded form where staff can easily report issues or share suggestions. An AI steering committee, including clinical, operational, and IT leaders, should review this feedback to determine whether challenges stem from training gaps, workflow inefficiencies, or tool limitations. Share success stories, such as reduced after-hours paperwork or faster referral processing, to build enthusiasm and momentum for expanding AI use.
Once initial workflows, like fax triage and referral management, are running smoothly, consider scaling AI to other areas. These might include prior authorization, intelligent scheduling, or AI-assisted documentation for low-acuity visits. By continuously refining and expanding AI applications, organizations can maximize its benefits while maintaining a focus on patient care and staff well-being.
Conclusion: Moving Forward with AI in Your Clinic
Bringing AI into your clinic doesn’t have to be overwhelming if you take a step-by-step approach. Start by evaluating your clinic’s readiness, put governance structures in place early, focus on high-impact administrative tasks, and only scale up after seeing measurable results. Interestingly, financial and operational leaders often rate their AI readiness at less than 3 out of 5. That’s why an objective readiness assessment is a smart first move. Once you’ve got a clear picture, establish a governance framework with defined roles, approval processes, and audit trails to protect your clinic as you grow. With these foundations set, you can turn your attention to implementing practical, high-value tasks.
Administrative workflows are a great place to start - especially low-risk, high-volume pre-visit processes like fax triage, referral tracking, and preparing prior authorizations. These areas consistently deliver fast results, helping to reduce staff burnout and improve patient flow without requiring major system changes. Tools such as Diagna's FAXFlo, Referral Manager, and Prior Auth Bot are perfect examples of solutions that integrate seamlessly with your existing EMR. They handle repetitive tasks while leaving room for human oversight in exceptions and clinical decisions. This approach ensures quick wins with minimal risk to patient care.
As previously mentioned, success with AI depends heavily on trust and transparency. Did you know that 79% of patients feel more at ease with AI when their clinicians take the time to explain how it’s being used? Staff also need targeted training to confidently use AI, verify outputs, and communicate its role to patients. By combining strong governance with ongoing education, you can foster a culture where AI is viewed as a helpful tool rather than a threat.
It’s also crucial to measure what matters. Identify 3–5 key success metrics - like minutes saved per visit, referral turnaround times, or faster prior authorization approvals - and track them carefully from pilot projects through to full implementation. Without clear baselines and goals, pilots can lead to vague outcomes, frustrating executives and stalling progress. The clinics that thrive treat AI adoption as an evolving process: test, measure, refine, and expand only what proves effective.
Clinics that embrace a thoughtful balance of caution and urgency - while investing in governance and workflow improvements - are most likely to benefit from AI while maintaining patient safety and staff confidence. Waiting too long can leave your clinic lagging behind competitors, but moving too quickly without safeguards can introduce unnecessary risks. The key to success lies in following these evidence-based steps.
FAQs
How can clinics ensure their AI systems comply with HIPAA regulations?
When incorporating AI into healthcare settings, clinics must take steps to align with HIPAA regulations. This starts with implementing secure data handling practices like encryption and strict access controls to keep patient information safe. Opting for AI tools specifically designed to meet regulatory requirements and ensuring they integrate smoothly with EMR systems adds another layer of protection for sensitive data.
Equally important is staff education - training employees on privacy protocols ensures everyone understands their role in safeguarding patient information. Regular audits of AI systems can also help identify potential vulnerabilities, keeping operations compliant and reinforcing patient trust.
What steps should clinics take to evaluate their readiness for adopting AI?
Clinics aiming to adopt AI should begin by examining their current workflows to pinpoint inefficiencies. For instance, delays in processing referrals or managing prior authorizations might signal areas ripe for improvement. Another key step is evaluating the compatibility of existing EMR systems to ensure they can support AI integration.
Equally important is preparing the staff for these changes. Offering thorough training can help ease the transition and build confidence in using new tools. Clinics must also prioritize compliance with regulations like HIPAA to protect patient data and maintain trust. These measures can lay the groundwork for smoothly incorporating AI into daily operations.
How can clinics accurately measure the ROI of AI in administrative workflows?
Clinics can assess the impact of AI on administrative tasks by focusing on measurable outcomes like time saved, revenue growth, and error reduction. For instance, tracking metrics such as saving 20+ hours per week, achieving a 15% boost in revenue, or improving accuracy to over 94% offers concrete evidence of AI's effectiveness.
Beyond these, clinics can monitor results like quicker document processing, fewer missed referrals, and streamlined workflows to better understand AI's role in improving operations. Regularly analyzing these key indicators allows clinics to make informed decisions and get the most out of their AI tools.
Related Blog Posts
AI is transforming outpatient clinics by automating tedious tasks like scheduling, fax sorting, and prior authorizations. While 71% of U.S. hospitals used AI in electronic health records by 2024, many clinics face hurdles like high costs, compliance concerns, and staff training gaps. This guide explains how clinics can prepare for AI, tackle barriers, and measure success with low-risk pilots in areas like document handling.
Key Takeaways:
Challenges: Financial concerns (47% cite unclear ROI), compliance issues (40% worry about HIPAA), and integration problems (77% struggle with legacy systems).
Solutions: Conduct readiness assessments, prioritize barriers, and start with manageable AI projects (e.g., automating fax triage).
Results: AI can cut administrative costs by 10–20% and save clinicians 3 hours weekly by reducing after-hours documentation.

AI Adoption Challenges and Benefits in Healthcare Clinics
AI in Healthcare 2025: November Breakthroughs for Your Practice
Evaluating Your Clinic's Readiness for AI
Before diving into AI adoption, it's essential to take stock of your clinic's current capabilities. A structured readiness assessment can provide a clear view of your strengths and weaknesses, helping you pinpoint areas that need attention. This evaluation lays the groundwork for the adjustments needed to ensure a smooth AI implementation.
Running a Readiness Assessment
To address the challenges of integrating AI, start by evaluating six key areas: EMR/EHR capabilities, data quality, people and skills, workflows and processes, technology infrastructure, and governance and compliance. For example, check if your EMR system supports APIs like HL7/FHIR and whether it can automatically update patient records.
Assess the quality of your data, focusing on areas like patient demographics, problem lists, and insurance details. Are referrals and prior authorizations arriving as structured, usable data, or are they messy faxes requiring manual intervention? Poor data quality is a common roadblock when rolling out AI solutions.
Next, evaluate your team's comfort level with digital tools such as patient portals or e-prescribing systems. Identifying a "clinical champion" to lead the way in piloting new workflows can be a game-changer, especially for smaller outpatient clinics that may lack specialized IT staff or robust training programs.
Your technology infrastructure is another critical area. Do you have secure internet connectivity, enough devices, and the capacity to support cloud-based tools while staying compliant with HIPAA requirements? Lastly, review your governance processes - whether formal or informal - for approving, monitoring, and auditing digital tools. A 2025 Black Book Research survey revealed that only 22% of hospital leaders could produce a complete AI audit trail within 30 days, showing that oversight gaps are still a major issue.
To simplify this process, create a checklist and score your clinic on a scale of 1 to 5 across these areas. This will give you a baseline readiness score and help identify where to invest before launching AI initiatives.
Mapping and Prioritizing Your Barriers
Once you've completed your readiness assessment, it’s time to map out the specific challenges your clinic faces. Organize a workshop with practice leaders, clinicians, front-office staff, and billing teams to identify perceived barriers. These challenges often fall into four categories:
Financial: Concerns over ROI, upfront costs, and subscription fees.
Technical: Limited EHR integration, poor data quality, or weak connectivity.
Workflow: Disruptions to existing processes and unclear task ownership.
Cultural: Fears about errors, liability, job security, or resistance to change.
Financial concerns often top the list, with unclear ROI and ongoing costs being major sticking points. Addressing these requires seamless integration into current workflows, transparency, and thorough training to build trust in AI tools.
Document these barriers using a spreadsheet or whiteboard, then prioritize them using a simple 2×2 grid. This grid compares the impact of each barrier on clinical or operational goals with the urgency of addressing it. High-impact, high-urgency issues - like revenue loss from delayed referrals or severe staff shortages - should take precedence. Lower-impact concerns, like minor interface glitches, can be addressed later. For many outpatient clinics, the most common challenges are workflow integration, data and infrastructure gaps, and financial uncertainty. Developing a focused action plan, such as standardizing referral intake processes or clarifying AI budgets with expected savings, can help tackle these issues before moving forward with a pilot.
Once you've identified and prioritized your barriers, set clear metrics to measure your progress.
Setting Measurable Success Metrics
Before rolling out any AI tool, establish baseline metrics that reflect both operational efficiency and financial performance. These metrics should address the financial, technical, and workflow challenges identified earlier. Consider tracking:
Average time from fax receipt to EMR indexing
Percentage of misfiled or lost faxes
Average referral processing time
Turnaround time for prior authorization requests
Total staff hours spent weekly on pre-visit administrative tasks
Additionally, monitor staff overtime related to administrative tasks, costs for temporary staff during peak periods, rates of denied or delayed claims due to missing documentation, and revenue losses from incomplete referrals.
Research shows that AI, when deployed effectively, can cut hospital operating costs by 10–20%, largely through administrative efficiencies. Setting SMART (Specific, Measurable, Achievable, Relevant, Time-bound) goals ensures you can track progress objectively. For instance, you might aim to reduce weekly staff hours spent on fax triage and indexing by 30% within six months of implementing AI, or cut referral processing times from five days to two. Similarly, you could target a 50% reduction in prior authorization turnaround times and a 40% drop in claims denials caused by missing documentation.
For pre-visit workflows, platforms like Diagna offer automation tools for fax triage, referral tracking, and prior authorization processing while integrating seamlessly with any EMR. As part of your readiness evaluation, review your current document volume, error rates in manual indexing, and the frequency of delays caused by incomplete referrals or authorizations. These baseline measurements will help you set realistic goals and demonstrate the ROI of your AI solution once it's live.
Establishing Governance, Compliance, and Trust
Once you've assessed your readiness and identified potential obstacles, the next step is to establish a strong governance framework that ensures your AI tools are safe, compliant, and trusted by your team. This structure connects your earlier evaluations to practical implementation, making sure AI is deployed responsibly and effectively.
Creating an AI Governance Framework
For an outpatient clinic, an effective governance framework typically focuses on five key areas: strategy and use-case selection, risk and safety oversight, data and privacy management, IT/security and integration, and training and change management. Assigning specific responsibilities to designated leads is essential.
Strategy and Use-Case Selection: A clinical or medical director, along with an operations leader, should handle strategy. Their role is to identify AI tools that align with the clinic's goals, whether it's improving patient access, enhancing care quality, or boosting revenue.
Risk and Safety Oversight: A clinician champion and a quality or safety representative should define what "safe use" looks like within your workflows. For example, staff should review all AI-generated document classifications before appointments or orders are triggered.
Data and Privacy Management: A compliance or privacy officer ensures HIPAA-compliant data handling, secures Business Associate Agreements (BAAs), and maintains audit trails for any AI tools interacting with protected health information.
IT/Security and Integration: An IT lead should evaluate vendors for security measures, system uptime, and electronic medical record (EMR) compatibility. They should also track model versions and system interfaces for audit purposes.
Training and Change Management: Clinical leadership and HR or education coordinators should provide role-specific training, outline approved workflows, and reinforce the importance of "human in the loop" oversight.
Clearly defining human responsibilities for each workflow step is critical. For instance, while AI-powered fax triage can classify and extract data, a referral coordinator should verify the classifications and key fields before creating orders. Specify which decisions AI can handle independently (e.g., assigning a fax to a "referrals" queue), which require human review (e.g., verifying provider details), and which are strictly reserved for clinicians (e.g., modifying a care plan). Many clinics streamline this process through an AI steering group that meets monthly to review proposals, monitor performance metrics, and approve changes before scaling.
Meeting Regulatory and Privacy Requirements
When implementing AI in pre-visit workflows, compliance with U.S. regulations like HIPAA, FTC and state consumer protection laws, and FDA guidance on software as a medical device (SaMD) is crucial. HIPAA governs the handling of protected health information (PHI), so any AI interacting with patient data must operate under a HIPAA-compliant framework with proper safeguards, access controls, and data minimization practices.
Administrative tools like fax classification generally fall outside FDA SaMD criteria since they don't provide diagnostic recommendations. However, ensure vendors position their software as operational support rather than clinical decision-making tools. The FDA's evolving guidance on AI/ML-enabled medical software applies if a tool influences clinical decisions or risk scores.
To maintain compliance, create a HIPAA checklist covering:
Legal Agreements: Secure a signed BAA outlining permitted PHI uses, breach notification timelines, subcontractor obligations, and data return or destruction policies.
Data Handling: Limit PHI usage to agreed purposes, with clear policies on retention, deletion, and disclosure during model training.
Security Controls: Implement encryption (in transit and at rest), role-based access controls, regular penetration testing, and incident response plans. Request third-party security certifications or audits.
Transparency and Logging: Maintain detailed logs of system access, model versions, configuration changes, and key automated actions to ensure auditability.
When evaluating vendors, use a standardized questionnaire to assess regulatory compliance, privacy protections, security measures, and operational fit. Key questions include whether the software qualifies as SaMD, what PHI it processes, whether data leaves the U.S., and how data minimization is handled. Request documentation on encryption standards, access controls, vulnerability management, and independent security assessments. For tools like Diagna's fax triage and prior authorization automation, confirm the platform operates under a BAA, integrates securely with your EMR, and provides exportable logs and admin dashboards for audits.
Building Staff and Clinician Confidence
Even the most robust governance framework won't succeed if your team doesn't trust the technology. Building confidence among clinicians and staff requires transparent communication, targeted training, and sharing validation data. A 2023 survey revealed that 78% of physicians emphasized the importance of transparency and training when using health AI, while 79% of patients reported feeling more comfortable when clinicians explained AI use.
Explain what the AI does, what it doesn't do, and where human oversight remains essential. For example, while AI may classify documents and extract data, a staff member should always verify these outputs before taking further action. Share validation data and real-world results - such as accuracy rates, time saved, and error reductions - to demonstrate the tool's benefits and limitations.
"Our software is built keeping in all regulatory guidelines from HIPAA. We base our workflows on top industry guidelines ensuring no compromise to data safety." – Diagna.ai
Involve clinicians during both design and implementation to ensure the tools meet practical needs. Focus on creating user-friendly interfaces that integrate seamlessly with EMR workflows, allowing data to sync directly into patient charts without manual effort. Starting with repetitive, high-volume tasks like fax triage, email sorting, and prior authorization form filling can help ease the transition. As staff see the AI delivering accurate results and saving significant time - potentially over 20 hours per week - they'll likely feel more comfortable expanding its use. Regularly reviewing performance dashboards to track usage, error rates, and any incidents ensures you can address concerns quickly and maintain trust.
Starting with High-Value, Low-Risk AI Solutions
Once you’ve established a strong governance framework, the next logical step is to kick off low-risk AI projects. The best starting point? Focus on administrative and pre-visit workflows that save time without impacting clinical decisions. Tasks like document handling, referral tracking, and prior authorization fit the bill perfectly. These processes are high-volume, follow clear rules, and take up a lot of staff time, but they carry minimal clinical risk when managed with proper oversight.
Automating Pre-Visit Workflows with AI
Using your governance framework as a foundation, start automating repetitive pre-visit tasks. U.S. clinics often see great results from three specific workflows: document triage, referral tracking, and prior authorization automation. Here's how each works:
Document triage: AI tools classify and extract critical data from faxes, such as lab results or referrals, and route them to the right folders in the EMR. This cuts sorting time in half and reduces routing errors.
Referral tracking: AI centralizes incoming referrals, tracks which patients have scheduled appointments, and flags those who haven’t, improving access and capturing revenue.
Prior authorization automation: AI pre-fills payer-specific forms using chart data, checks for missing details, and tracks submission progress, reducing turnaround times by 30–50%.
Diagna's tools - FAXFlo, Referral Manager, and Prior Auth Bot - integrate directly with your EMR, pushing structured data into the right fields and queues. This eliminates the need for staff to retype information or toggle between systems. AI accuracy in processing clinical documents has reached 94%, matching human performance and ensuring same-day document handling.
"Our AI integrates around your workflows, not the other way around - no matter which EMR you use." – Diagna.ai
Testing AI with Small-Scale Pilots
A smart way to introduce AI is through small, controlled pilots. Begin by defining clear boundaries: choose a single workflow (like handling inbound referral faxes), limit it to one department, and run it for 60–90 days with a manageable volume, such as up to 200 faxes daily. Before starting, collect baseline data, including processing time per item, staff hours spent, error rates, and the time from referral receipt to appointment scheduling. Identify potential issues, like misrouted faxes or missed referrals, and establish clear escalation procedures.
Provide brief training sessions and simple guides to help staff understand how to use the AI and handle exceptions. Assign specific clinical or operational owners, as well as IT/data leads, to oversee the process and address any issues like misclassifications or downtime. Hold weekly reviews to analyze data, gather feedback, and make necessary adjustments. At the end of the pilot, compare the results to your baseline, evaluate staff feedback, and decide whether to stop, extend, or expand the project. If the pilot meets success criteria, you can scale the solution to other workflows.
Connecting AI with Your EMR System
For AI to be effective, it needs to work seamlessly with your EMR. This means AI outputs should appear in the same screens and queues your staff already use, avoiding the need for separate portals that create extra work. Collaborate with your vendor and EMR team to use existing interfaces and APIs - like HL7 or FHIR - to ensure AI outputs are stored as structured data, correctly linked to the right patient and provider. Route AI-generated tasks to established work queues (e.g., "referral work queue" or "prior auth work queue") so staff can manage them within familiar workflows.
To enhance tracking and quality oversight, configure specific fields populated by AI - such as referral reasons, referring providers, payers, and authorization IDs. These fields should be searchable and reportable. Before going live, test the integration in a controlled environment to ensure proper patient matching, document routing, and user permissions.
Training Staff and Scaling AI Adoption
Providing Role-Specific AI Training
To successfully integrate AI tools into healthcare workflows, it's crucial to provide tailored training for each role. Front-desk staff, clinicians, and billing coordinators all interact with AI differently, so their training should reflect these unique needs. For instance, front-desk and access teams need hands-on experience with AI tools for scheduling, patient intake, and insurance verification. Clinicians must focus on interpreting AI outputs, understanding its limitations (like occasional inaccuracies), and maintaining clinical judgment to avoid over-reliance on automation. Billing coordinators, on the other hand, should master AI features like claim scrubbing, coding suggestions, and automated prior authorization workflows, with a strong emphasis on compliance and escalation procedures.
A tiered micro-learning approach works well here. Start with 20–30 minute onboarding sessions tailored to each role, followed by short refresher modules every three to six months. Use a mix of formats, such as live demonstrations within the EMR, quick e-learning modules, and job aids integrated into daily workflows. To minimize disruptions, schedule these sessions during protected times like monthly staff meetings or quick team huddles. Designating "AI super-users" in each role can also provide just-in-time peer support and coaching.
Training must also address key concerns like safety, privacy, and the scope of AI use. Staff should understand how patient data is protected, what information is shared with vendors, and how AI outputs are monitored. Hands-on exercises - like comparing manual referral triage with AI-driven automation - can help staff see the practical benefits, such as time savings, while reinforcing that final decisions remain human-led. A Philips survey revealed that 79% of patients felt more comfortable when clinicians clearly explained how AI was being used. Leaders should emphasize that AI is designed to reduce administrative burdens, not replace staff, which can help lower burnout and improve job satisfaction.
Updating Policies and Workflows
Effective AI adoption requires updated policies and workflows that align with new practices. Start by clearly defining approved AI use cases, mandatory human reviews, and role-based responsibilities. Document how AI outputs will integrate into the EMR, specifying where AI-generated notes or triaged documents will appear, how they’ll be labeled, and the escalation process for discrepancies. Establish robust audit and logging practices - an area where only about 22% of hospitals currently feel confident.
Job descriptions should also be updated to include expectations around AI tool usage, performance monitoring, and ongoing training participation. Collaborate with vendors and IT teams to ensure AI tools seamlessly integrate with existing systems, like EMRs and task queues. For example, AI-based fax management should route triaged documents directly into the same EMR work queues staff already use, eliminating the need for multiple logins or duplicate data entry. Poorly integrated tools can disrupt workflows and lead to inefficiencies, even when the AI itself performs accurately.
Tracking Performance and Expanding Use Cases
Once staff are trained and workflows are updated, ongoing performance tracking becomes essential. Monitoring key performance indicators (KPIs) helps ensure AI adoption improves efficiency without compromising patient care. Focus on metrics like referral-to-appointment times, the speed of fax/referral processing (e.g., percentage completed within 24–48 hours), prior authorization turnaround times, denied claims reduction, and staff overtime costs. Studies suggest well-implemented AI can cut hospital operating costs by 10–20%. Additionally, track experiential metrics like staff satisfaction, burnout levels, appointment wait times, and call-back speeds. Establish baseline metrics before AI implementation and review them regularly - such as 60 to 90 days post-launch - to identify areas needing further training or adjustments.
To refine processes, create structured feedback loops. Use tools like brief pulse surveys, periodic focus groups, or an EMR-embedded form where staff can easily report issues or share suggestions. An AI steering committee, including clinical, operational, and IT leaders, should review this feedback to determine whether challenges stem from training gaps, workflow inefficiencies, or tool limitations. Share success stories, such as reduced after-hours paperwork or faster referral processing, to build enthusiasm and momentum for expanding AI use.
Once initial workflows, like fax triage and referral management, are running smoothly, consider scaling AI to other areas. These might include prior authorization, intelligent scheduling, or AI-assisted documentation for low-acuity visits. By continuously refining and expanding AI applications, organizations can maximize its benefits while maintaining a focus on patient care and staff well-being.
Conclusion: Moving Forward with AI in Your Clinic
Bringing AI into your clinic doesn’t have to be overwhelming if you take a step-by-step approach. Start by evaluating your clinic’s readiness, put governance structures in place early, focus on high-impact administrative tasks, and only scale up after seeing measurable results. Interestingly, financial and operational leaders often rate their AI readiness at less than 3 out of 5. That’s why an objective readiness assessment is a smart first move. Once you’ve got a clear picture, establish a governance framework with defined roles, approval processes, and audit trails to protect your clinic as you grow. With these foundations set, you can turn your attention to implementing practical, high-value tasks.
Administrative workflows are a great place to start - especially low-risk, high-volume pre-visit processes like fax triage, referral tracking, and preparing prior authorizations. These areas consistently deliver fast results, helping to reduce staff burnout and improve patient flow without requiring major system changes. Tools such as Diagna's FAXFlo, Referral Manager, and Prior Auth Bot are perfect examples of solutions that integrate seamlessly with your existing EMR. They handle repetitive tasks while leaving room for human oversight in exceptions and clinical decisions. This approach ensures quick wins with minimal risk to patient care.
As previously mentioned, success with AI depends heavily on trust and transparency. Did you know that 79% of patients feel more at ease with AI when their clinicians take the time to explain how it’s being used? Staff also need targeted training to confidently use AI, verify outputs, and communicate its role to patients. By combining strong governance with ongoing education, you can foster a culture where AI is viewed as a helpful tool rather than a threat.
It’s also crucial to measure what matters. Identify 3–5 key success metrics - like minutes saved per visit, referral turnaround times, or faster prior authorization approvals - and track them carefully from pilot projects through to full implementation. Without clear baselines and goals, pilots can lead to vague outcomes, frustrating executives and stalling progress. The clinics that thrive treat AI adoption as an evolving process: test, measure, refine, and expand only what proves effective.
Clinics that embrace a thoughtful balance of caution and urgency - while investing in governance and workflow improvements - are most likely to benefit from AI while maintaining patient safety and staff confidence. Waiting too long can leave your clinic lagging behind competitors, but moving too quickly without safeguards can introduce unnecessary risks. The key to success lies in following these evidence-based steps.
FAQs
How can clinics ensure their AI systems comply with HIPAA regulations?
When incorporating AI into healthcare settings, clinics must take steps to align with HIPAA regulations. This starts with implementing secure data handling practices like encryption and strict access controls to keep patient information safe. Opting for AI tools specifically designed to meet regulatory requirements and ensuring they integrate smoothly with EMR systems adds another layer of protection for sensitive data.
Equally important is staff education - training employees on privacy protocols ensures everyone understands their role in safeguarding patient information. Regular audits of AI systems can also help identify potential vulnerabilities, keeping operations compliant and reinforcing patient trust.
What steps should clinics take to evaluate their readiness for adopting AI?
Clinics aiming to adopt AI should begin by examining their current workflows to pinpoint inefficiencies. For instance, delays in processing referrals or managing prior authorizations might signal areas ripe for improvement. Another key step is evaluating the compatibility of existing EMR systems to ensure they can support AI integration.
Equally important is preparing the staff for these changes. Offering thorough training can help ease the transition and build confidence in using new tools. Clinics must also prioritize compliance with regulations like HIPAA to protect patient data and maintain trust. These measures can lay the groundwork for smoothly incorporating AI into daily operations.
How can clinics accurately measure the ROI of AI in administrative workflows?
Clinics can assess the impact of AI on administrative tasks by focusing on measurable outcomes like time saved, revenue growth, and error reduction. For instance, tracking metrics such as saving 20+ hours per week, achieving a 15% boost in revenue, or improving accuracy to over 94% offers concrete evidence of AI's effectiveness.
Beyond these, clinics can monitor results like quicker document processing, fewer missed referrals, and streamlined workflows to better understand AI's role in improving operations. Regularly analyzing these key indicators allows clinics to make informed decisions and get the most out of their AI tools.