AI Referral Analytics: Benefits for Clinics Explained
Healthcare Technology
Healthcare Technology
AI referral analytics reduces admin time, cuts referral leakage, speeds authorizations, and improves patient care and clinic revenue.
AI referral analytics reduces admin time, cuts referral leakage, speeds authorizations, and improves patient care and clinic revenue.

Did you know? 76% of physician referrals still rely on outdated methods like paper mail and fax, leading to inefficiencies like 46% of referrals never becoming scheduled appointments. This results in hospitals losing up to $971,000 per physician annually due to referral leakage.
AI referral analytics is changing this. By automating processes like data entry, insurance verification, and document sorting, these tools reduce errors, save time, and improve patient care. Here’s what AI-powered systems can deliver:
70% less time spent on administrative tasks like transcribing referrals.
50% productivity boost for staff through automated insights.
25% shorter call handling times for patient follow-ups.
Compared to manual systems, AI solutions offer faster processing, better accuracy, and the ability to handle more referrals without adding staff. For example, one clinic avoided hiring an extra employee by adopting AI tools, while another reduced prior authorization times from 5 days to under 24 hours.
Clinics using AI see fewer delays, better tracking, and higher revenue retention. Starting small - like automating one department - lets clinics test these tools before scaling up. The result? Faster care, reduced no-shows, and fewer gaps in patient follow-through.
1. Traditional Referral Analytics
Accuracy and Data Quality
Traditional referral analytics heavily rely on manual processes - think faxes, printed forms, emails, spreadsheets, and electronic health record (EHR) messages. While this approach allows physicians to draw on personal relationships and clinical judgment, it struggles with accuracy. Research shows that manual methods only hit 52.2% accuracy and 34% specificity when filtering out unnecessary referrals.
The problems don’t stop there. Nearly 19.8% of paper referrals lack clear reasoning, and almost half go untracked. Even more concerning, 68% of specialists report receiving no preliminary information before patient visits. Elisabeth Buford, an industry expert, summed it up:
"It's clear: the traditional referral process is broken." - Elisabeth Buford
These gaps in accuracy and data handling only add to the delays in the referral process.
Speed and Turnaround Time
Communication delays are a major flaw in traditional systems. In 25% of cases, specialist feedback letters arrive too late to influence clinical decisions. Even with shared electronic medical records, specialists fail to send feedback within seven days in 36% of cases. Unsurprisingly, half of referring physicians are dissatisfied with the timeliness of specialist responses.
The administrative workload makes things worse. Nurses and medical assistants dedicate 20 hours per physician each week to administrative tasks, while providers themselves spend another 13 hours on manual prior authorizations. Once a referral is sent, the process often becomes a black hole - providers don’t know if the specialist received it, whether the patient scheduled an appointment, or what the outcome was.
Scalability and Operational Load
The sheer volume of referrals overwhelms traditional systems. In the U.S. alone, ambulatory settings generate more than 100 million subspecialist referrals annually. Manual processes simply can’t keep up. The result? Up to 50% of referrals are never completed, and 50-65% experience “leakage” - patients either see a different provider than recommended or abandon the referral altogether.
The financial losses tied to these inefficiencies are staggering. Referral leakage costs each physician between $821,000 and $971,000 in annual hospital revenue. For health systems with 100 affiliated providers, this translates to $78 million to $97 million in lost revenue every year. What’s driving this? A lack of reliable specialist information, cited by 87% of physicians, leads to 19.7 million clinically inappropriate referrals in the U.S. annually.
Accelerate referral processing with AI guided triage
2. AI Referral Analytics
AI is reshaping referral analytics, addressing longstanding challenges with improved precision and speed.
Accuracy and Data Quality
AI excels at turning unstructured data into organized, structured formats. Tools powered by Optical Character Recognition (OCR) and Natural Language Processing (NLP) can instantly extract details from handwritten notes, faxes, and PDFs - eliminating errors caused by manual data entry. Instead of relying on incomplete paper referrals, AI systems automatically sort and classify documents, making them easier and faster for care teams to review.
The results speak for themselves. In Brazil, an AI model designed to manage referrals achieved an accuracy of 0.716, outperforming human reviewers by almost 20%. This system authorized 22,000 out of 72,000 monthly referrals in Rio Grande do Sul, streamlining specialist consultations and lightening the workload. Healthcare providers using AI-powered OCR and data extraction have also reported cutting manual processing time by up to 70%.
Speed and Turnaround Time
By automating tasks like data conversion, form completion, and document sorting, AI slashes referral turnaround times. Processes that used to take 48–72 hours can now be completed in under 24 hours. Similarly, prior authorization workflows that once stretched over 3–5 days are now often completed within a single day thanks to AI. For example, one U.S. hospital network reduced its authorization turnaround from five days to less than 24 hours after adopting AI referral automation.
"Automating the referral process reduces the reliance on manual tasks, such as filling out forms, making phone calls, and sending faxes." – Bruce Orcutt, Chief Marketing Officer, ABBYY
AI also simplifies clinical histories into concise summaries, ensuring specialists quickly get the information they need . Automated follow-ups further ensure patients stay on track with their care, reducing no-shows and maintaining continuity . By automating tasks like data entry and document management, healthcare teams can save 10–20 administrative hours each week.
Scalability and Operational Load
AI systems can handle large referral volumes without requiring additional staff. A study of 17,378 ENT referrals from 2019 to 2022 demonstrated how AI could automate categorization based on Clinical Prioritization Criteria. Another study using machine learning for referral triage achieved a micro F1 score of 0.98, showcasing its scalability and efficiency.
These systems also bring operational benefits, such as reducing transcription time, improving productivity through actionable insights, and shortening call handling times. Platforms like Diagna's Referral Manager streamline tasks like document triage, referral tracking, and prior authorization, integrating seamlessly with existing EMR systems to cut down on manual work. Additionally, AI referral systems can reduce information loss and patient migration by up to 20% within six months. These efficiencies directly translate to better clinical performance and financial results.
Clinical and Business Outcomes
The operational improvements driven by AI lead to faster processes and better care quality. One healthcare provider using AI referral management saw a 30% drop in referral delays and significantly faster processing times. AI can even predict when a referral might be needed based on patient data, sending timely alerts to clinicians and reducing the chance of missing critical referrals.
"More than just a productivity tool, it's a strategic asset that improves the quality, timeliness, and cost-effectiveness of care transitions." – Cabot Solutions
Pros and Cons
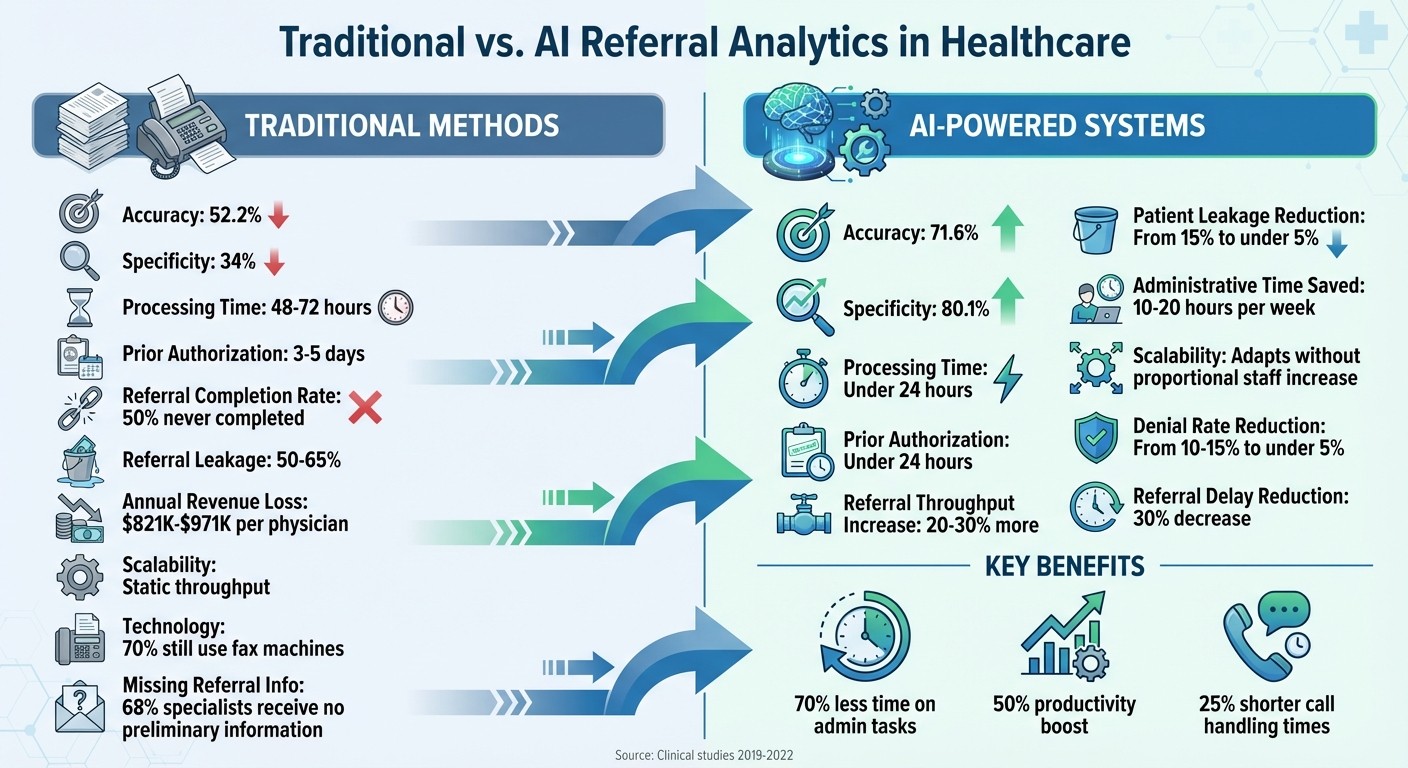
Traditional vs AI Referral Analytics: Key Performance Metrics Comparison
When comparing traditional and AI-powered referral analytics, it’s clear that each approach comes with its own set of strengths and weaknesses. These trade-offs play a crucial role in how clinics manage patient referrals, helping healthcare administrators decide the best fit for their workflows.
Traditional methods have a notable downside: they deliver only about 52.2% accuracy and relatively low specificity. This often results in unnecessary authorizations and wasted resources, which can strain both time and budgets.
On the other hand, AI-powered systems bring a significant boost in performance. These systems achieve an overall accuracy of 71.6% and an 80.1% specificity rate, meaning fewer false positives and unnecessary referrals. Additionally, automation and faster data processing allow staff to handle 20–30% more referrals, making the workflow more efficient. However, this increased efficiency comes with a trade-off: a higher false negative rate, which could delay critical care for some patients.
Scalability is another key area where the two methods diverge. Traditional systems often hit a ceiling, as referral throughput remains static regardless of increased workload. For instance, over 70% of providers in North America still rely on fax machines, and primary care visits account for around 70% of referrals. These outdated processes can easily become overwhelmed. In contrast, AI solutions are built to adapt and scale without requiring a proportional increase in staff, making them a more flexible option.
Given these factors, many clinics are exploring a hybrid approach. By combining AI automation with targeted human oversight, healthcare providers can leverage the strengths of both methods while minimizing their shortcomings.
Conclusion
The difference between traditional methods and AI-powered referral analytics is striking. Traditional approaches, often relying on manual processes and disjointed workflows, are prone to errors and delays. For instance, it typically takes 48–72 hours to process referrals and 3–5 days for prior authorizations. In contrast, AI systems streamline these tasks, reducing processing times to under 24 hours while achieving an impressive 80.1% specificity in identifying cases that don’t need further approval . These advancements in speed and accuracy translate into clear operational improvements.
For clinics considering AI adoption, the potential benefits are measurable and impactful. AI referral analytics can reduce patient leakage from around 15% to under 5%, save 10–20 hours of administrative work per week, and boost referral throughput by 20–30%. Additionally, denial rates drop significantly, from 10–15% to less than 5%, thanks to more accurate and complete documentation.
Implementing AI doesn’t have to be overwhelming. Clinics can start small by addressing specific pain points in their referral management process. Begin by mapping out current workflows and pinpointing bottlenecks - like fax backlogs, delays in authorizations, or gaps in tracking referrals. Partnering with a HIPAA-compliant vendor that integrates smoothly with existing electronic medical record (EMR) systems allows clinics to pilot AI tools in one department or specialty. During this trial phase, key performance metrics - such as turnaround times, referral completion rates, and administrative hours saved - can be tracked to evaluate success before expanding the system across the organization.
FAQs
How does AI-powered referral analytics enhance accuracy and speed in managing referrals?
AI-driven referral analytics brings a new level of precision to handling patient data. By automatically extracting, verifying, and summarizing referral information, it minimizes the chance of human error. This ensures that data is processed accurately, offering a more dependable system for managing referrals.
On top of that, it dramatically enhances efficiency by processing referrals in mere seconds. This quick triage system simplifies workflows and cuts down on processing times, allowing clinics to manage referrals more effectively. The result? Time saved for both healthcare staff and patients.
How can clinics financially benefit from using AI referral analytics?
AI referral analytics offers clinics a way to cut costs by automating time-consuming tasks and reducing errors in referral workflows. By simplifying these processes, clinics can lower administrative burdens and improve accuracy, leading to fewer delays and mistakes.
On top of that, faster referral processing means clinics can book more patient appointments, opening the door to greater revenue. With these efficiencies in place, staff can shift their attention to more impactful responsibilities, boosting both financial performance and overall operations.
How can clinics adopt AI referral analytics without disrupting their current workflows?
Clinics can ease into using AI for referral analytics by taking a step-by-step approach. Start by pinpointing issues in your current referral process - think delays or tedious manual tasks. Then, choose an AI tool that works well with your existing electronic medical records (EMR) system. A good way to begin is with a small pilot project, such as automating fax triage. This can help cut down on manual work and improve efficiency without requiring a complete system overhaul.
After seeing success in the initial phase, you can gradually add more features. For example, you might introduce advanced analytics, automated scheduling, or tools for handling prior authorizations. Make sure to provide staff with clear, focused training and keep an eye on key metrics like faster processing times or better referral tracking. This way, you can showcase the benefits early on while keeping your operations running smoothly.
Related Blog Posts
Did you know? 76% of physician referrals still rely on outdated methods like paper mail and fax, leading to inefficiencies like 46% of referrals never becoming scheduled appointments. This results in hospitals losing up to $971,000 per physician annually due to referral leakage.
AI referral analytics is changing this. By automating processes like data entry, insurance verification, and document sorting, these tools reduce errors, save time, and improve patient care. Here’s what AI-powered systems can deliver:
70% less time spent on administrative tasks like transcribing referrals.
50% productivity boost for staff through automated insights.
25% shorter call handling times for patient follow-ups.
Compared to manual systems, AI solutions offer faster processing, better accuracy, and the ability to handle more referrals without adding staff. For example, one clinic avoided hiring an extra employee by adopting AI tools, while another reduced prior authorization times from 5 days to under 24 hours.
Clinics using AI see fewer delays, better tracking, and higher revenue retention. Starting small - like automating one department - lets clinics test these tools before scaling up. The result? Faster care, reduced no-shows, and fewer gaps in patient follow-through.
1. Traditional Referral Analytics
Accuracy and Data Quality
Traditional referral analytics heavily rely on manual processes - think faxes, printed forms, emails, spreadsheets, and electronic health record (EHR) messages. While this approach allows physicians to draw on personal relationships and clinical judgment, it struggles with accuracy. Research shows that manual methods only hit 52.2% accuracy and 34% specificity when filtering out unnecessary referrals.
The problems don’t stop there. Nearly 19.8% of paper referrals lack clear reasoning, and almost half go untracked. Even more concerning, 68% of specialists report receiving no preliminary information before patient visits. Elisabeth Buford, an industry expert, summed it up:
"It's clear: the traditional referral process is broken." - Elisabeth Buford
These gaps in accuracy and data handling only add to the delays in the referral process.
Speed and Turnaround Time
Communication delays are a major flaw in traditional systems. In 25% of cases, specialist feedback letters arrive too late to influence clinical decisions. Even with shared electronic medical records, specialists fail to send feedback within seven days in 36% of cases. Unsurprisingly, half of referring physicians are dissatisfied with the timeliness of specialist responses.
The administrative workload makes things worse. Nurses and medical assistants dedicate 20 hours per physician each week to administrative tasks, while providers themselves spend another 13 hours on manual prior authorizations. Once a referral is sent, the process often becomes a black hole - providers don’t know if the specialist received it, whether the patient scheduled an appointment, or what the outcome was.
Scalability and Operational Load
The sheer volume of referrals overwhelms traditional systems. In the U.S. alone, ambulatory settings generate more than 100 million subspecialist referrals annually. Manual processes simply can’t keep up. The result? Up to 50% of referrals are never completed, and 50-65% experience “leakage” - patients either see a different provider than recommended or abandon the referral altogether.
The financial losses tied to these inefficiencies are staggering. Referral leakage costs each physician between $821,000 and $971,000 in annual hospital revenue. For health systems with 100 affiliated providers, this translates to $78 million to $97 million in lost revenue every year. What’s driving this? A lack of reliable specialist information, cited by 87% of physicians, leads to 19.7 million clinically inappropriate referrals in the U.S. annually.
Accelerate referral processing with AI guided triage
2. AI Referral Analytics
AI is reshaping referral analytics, addressing longstanding challenges with improved precision and speed.
Accuracy and Data Quality
AI excels at turning unstructured data into organized, structured formats. Tools powered by Optical Character Recognition (OCR) and Natural Language Processing (NLP) can instantly extract details from handwritten notes, faxes, and PDFs - eliminating errors caused by manual data entry. Instead of relying on incomplete paper referrals, AI systems automatically sort and classify documents, making them easier and faster for care teams to review.
The results speak for themselves. In Brazil, an AI model designed to manage referrals achieved an accuracy of 0.716, outperforming human reviewers by almost 20%. This system authorized 22,000 out of 72,000 monthly referrals in Rio Grande do Sul, streamlining specialist consultations and lightening the workload. Healthcare providers using AI-powered OCR and data extraction have also reported cutting manual processing time by up to 70%.
Speed and Turnaround Time
By automating tasks like data conversion, form completion, and document sorting, AI slashes referral turnaround times. Processes that used to take 48–72 hours can now be completed in under 24 hours. Similarly, prior authorization workflows that once stretched over 3–5 days are now often completed within a single day thanks to AI. For example, one U.S. hospital network reduced its authorization turnaround from five days to less than 24 hours after adopting AI referral automation.
"Automating the referral process reduces the reliance on manual tasks, such as filling out forms, making phone calls, and sending faxes." – Bruce Orcutt, Chief Marketing Officer, ABBYY
AI also simplifies clinical histories into concise summaries, ensuring specialists quickly get the information they need . Automated follow-ups further ensure patients stay on track with their care, reducing no-shows and maintaining continuity . By automating tasks like data entry and document management, healthcare teams can save 10–20 administrative hours each week.
Scalability and Operational Load
AI systems can handle large referral volumes without requiring additional staff. A study of 17,378 ENT referrals from 2019 to 2022 demonstrated how AI could automate categorization based on Clinical Prioritization Criteria. Another study using machine learning for referral triage achieved a micro F1 score of 0.98, showcasing its scalability and efficiency.
These systems also bring operational benefits, such as reducing transcription time, improving productivity through actionable insights, and shortening call handling times. Platforms like Diagna's Referral Manager streamline tasks like document triage, referral tracking, and prior authorization, integrating seamlessly with existing EMR systems to cut down on manual work. Additionally, AI referral systems can reduce information loss and patient migration by up to 20% within six months. These efficiencies directly translate to better clinical performance and financial results.
Clinical and Business Outcomes
The operational improvements driven by AI lead to faster processes and better care quality. One healthcare provider using AI referral management saw a 30% drop in referral delays and significantly faster processing times. AI can even predict when a referral might be needed based on patient data, sending timely alerts to clinicians and reducing the chance of missing critical referrals.
"More than just a productivity tool, it's a strategic asset that improves the quality, timeliness, and cost-effectiveness of care transitions." – Cabot Solutions
Pros and Cons

Traditional vs AI Referral Analytics: Key Performance Metrics Comparison
When comparing traditional and AI-powered referral analytics, it’s clear that each approach comes with its own set of strengths and weaknesses. These trade-offs play a crucial role in how clinics manage patient referrals, helping healthcare administrators decide the best fit for their workflows.
Traditional methods have a notable downside: they deliver only about 52.2% accuracy and relatively low specificity. This often results in unnecessary authorizations and wasted resources, which can strain both time and budgets.
On the other hand, AI-powered systems bring a significant boost in performance. These systems achieve an overall accuracy of 71.6% and an 80.1% specificity rate, meaning fewer false positives and unnecessary referrals. Additionally, automation and faster data processing allow staff to handle 20–30% more referrals, making the workflow more efficient. However, this increased efficiency comes with a trade-off: a higher false negative rate, which could delay critical care for some patients.
Scalability is another key area where the two methods diverge. Traditional systems often hit a ceiling, as referral throughput remains static regardless of increased workload. For instance, over 70% of providers in North America still rely on fax machines, and primary care visits account for around 70% of referrals. These outdated processes can easily become overwhelmed. In contrast, AI solutions are built to adapt and scale without requiring a proportional increase in staff, making them a more flexible option.
Given these factors, many clinics are exploring a hybrid approach. By combining AI automation with targeted human oversight, healthcare providers can leverage the strengths of both methods while minimizing their shortcomings.
Conclusion
The difference between traditional methods and AI-powered referral analytics is striking. Traditional approaches, often relying on manual processes and disjointed workflows, are prone to errors and delays. For instance, it typically takes 48–72 hours to process referrals and 3–5 days for prior authorizations. In contrast, AI systems streamline these tasks, reducing processing times to under 24 hours while achieving an impressive 80.1% specificity in identifying cases that don’t need further approval . These advancements in speed and accuracy translate into clear operational improvements.
For clinics considering AI adoption, the potential benefits are measurable and impactful. AI referral analytics can reduce patient leakage from around 15% to under 5%, save 10–20 hours of administrative work per week, and boost referral throughput by 20–30%. Additionally, denial rates drop significantly, from 10–15% to less than 5%, thanks to more accurate and complete documentation.
Implementing AI doesn’t have to be overwhelming. Clinics can start small by addressing specific pain points in their referral management process. Begin by mapping out current workflows and pinpointing bottlenecks - like fax backlogs, delays in authorizations, or gaps in tracking referrals. Partnering with a HIPAA-compliant vendor that integrates smoothly with existing electronic medical record (EMR) systems allows clinics to pilot AI tools in one department or specialty. During this trial phase, key performance metrics - such as turnaround times, referral completion rates, and administrative hours saved - can be tracked to evaluate success before expanding the system across the organization.
FAQs
How does AI-powered referral analytics enhance accuracy and speed in managing referrals?
AI-driven referral analytics brings a new level of precision to handling patient data. By automatically extracting, verifying, and summarizing referral information, it minimizes the chance of human error. This ensures that data is processed accurately, offering a more dependable system for managing referrals.
On top of that, it dramatically enhances efficiency by processing referrals in mere seconds. This quick triage system simplifies workflows and cuts down on processing times, allowing clinics to manage referrals more effectively. The result? Time saved for both healthcare staff and patients.
How can clinics financially benefit from using AI referral analytics?
AI referral analytics offers clinics a way to cut costs by automating time-consuming tasks and reducing errors in referral workflows. By simplifying these processes, clinics can lower administrative burdens and improve accuracy, leading to fewer delays and mistakes.
On top of that, faster referral processing means clinics can book more patient appointments, opening the door to greater revenue. With these efficiencies in place, staff can shift their attention to more impactful responsibilities, boosting both financial performance and overall operations.
How can clinics adopt AI referral analytics without disrupting their current workflows?
Clinics can ease into using AI for referral analytics by taking a step-by-step approach. Start by pinpointing issues in your current referral process - think delays or tedious manual tasks. Then, choose an AI tool that works well with your existing electronic medical records (EMR) system. A good way to begin is with a small pilot project, such as automating fax triage. This can help cut down on manual work and improve efficiency without requiring a complete system overhaul.
After seeing success in the initial phase, you can gradually add more features. For example, you might introduce advanced analytics, automated scheduling, or tools for handling prior authorizations. Make sure to provide staff with clear, focused training and keep an eye on key metrics like faster processing times or better referral tracking. This way, you can showcase the benefits early on while keeping your operations running smoothly.